Events
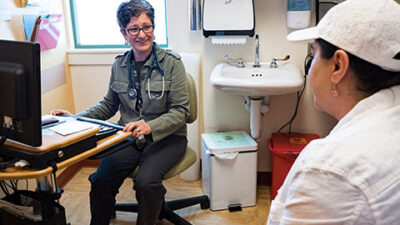
We host in-person and online events to bring stakeholders together to find solutions, spread knowledge, and create the impetus for change in California’s health care system. When available, we post video recordings of our events as well as presentation materials, so you’ll never miss a thing.