This case study is part of the CIN series Stories from the Field: Social Needs Screening and Referral Models.1 Its resources include the tools Senior Care Action Network Health Plan used to take action across its systems.
SCAN Health Plan was founded in 1977 as a social service organization dedicated to keeping seniors healthy and independent. Two years later, the state of California launched the Multipurpose Senior Services Program (MSSP) to provide care management and support services to chronically ill seniors with low incomes. SCAN was one of eight organizations selected to participate; today it’s the largest of the state’s MSSP sites. In 1985, SCAN piloted the Social Health Maintenance Organization (SHMO), a plan that featured a mix of community-based services and medical care. While SHMOs were discontinued in 2004, SCAN continued to offer Medicare Advantage plans and, in 2008, added a Special Needs Plan (SNP) specific to people who qualify for both Medicaid and Medicare (known as dual-eligible people).
From its roots as a social services organization and long experience serving seniors with low incomes, the health plan recognized that dual-eligible members were disproportionately affected by social risk factors such as poverty, social isolation, and homelessness. In order to improve clinical outcomes and control the total cost of care, SCAN began assessing and addressing the social needs of members in the SNP, including dual-eligible members, institutionalized members, and members with disabling chronic conditions.
In 2018, SCAN expanded its social needs screening and referral program to include standardized assessments and referrals for all health plan members. It focused on the following areas:
- Incorporating standardized social needs questions into its health risk assessment (HRA) for non-special needs members (known as the HRA for All)
- Contracting with a vendor called Aunt Bertha to develop and implement an online community resource directory and referral system
This case study will examine lessons from SCAN Health Plan’s work around social needs that impact health, with a focus on the tools it implemented to screen patients for social needs and electronically refer them to community organizations.
Organization Overview
SCAN Health Plan is a Medicare Advantage Health Maintenance Organization in California. It also contracts with the California Department of Health Care Services to provide health care coverage to dual-eligible members. SCAN currently provides coverage to more than 200,000 members in ten counties in the state. More than 15,000 of those members are dual eligible.
Independence at Home, a SCAN community service, provides care management and other vital services and support to seniors and their caregivers, regardless of plan membership. This direct connection gives the plan in-depth knowledge about the needs of the communities it serves as well as the availability of local resources. Independence at Home also offers education programs, community funding, volunteer opportunities, and other community services throughout SCAN’s California service area.
| organization | SCAN health plan |
|---|---|
| Project | Standardize social needs screening and referral process, including: – Incorporating standardized social needs questions into the HRA for non-special needs members (called HRA for All) – Contracting with Aunt Bertha to implement community resource directory and referral system |
| Implementation Status | – Screening: SCAN began incorporating social needs questions into its HRA for All three years ago. – Referrals: SCAN contracted with Aunt Bertha and began implementing its community resource directory and referral system in early 2018. – 2019 marks Year 3 of SCAN’s work spreading its social needs screening and referral process to its entire member population. |
| Tools and Methods Tested | Health risk assessment (includes metrics related to social needs); Aunt Bertha screening and referral system |
| Funding Source(s) | This work is funded through SCAN Health Plan. |
Social Needs Screening and Referrals Workflow
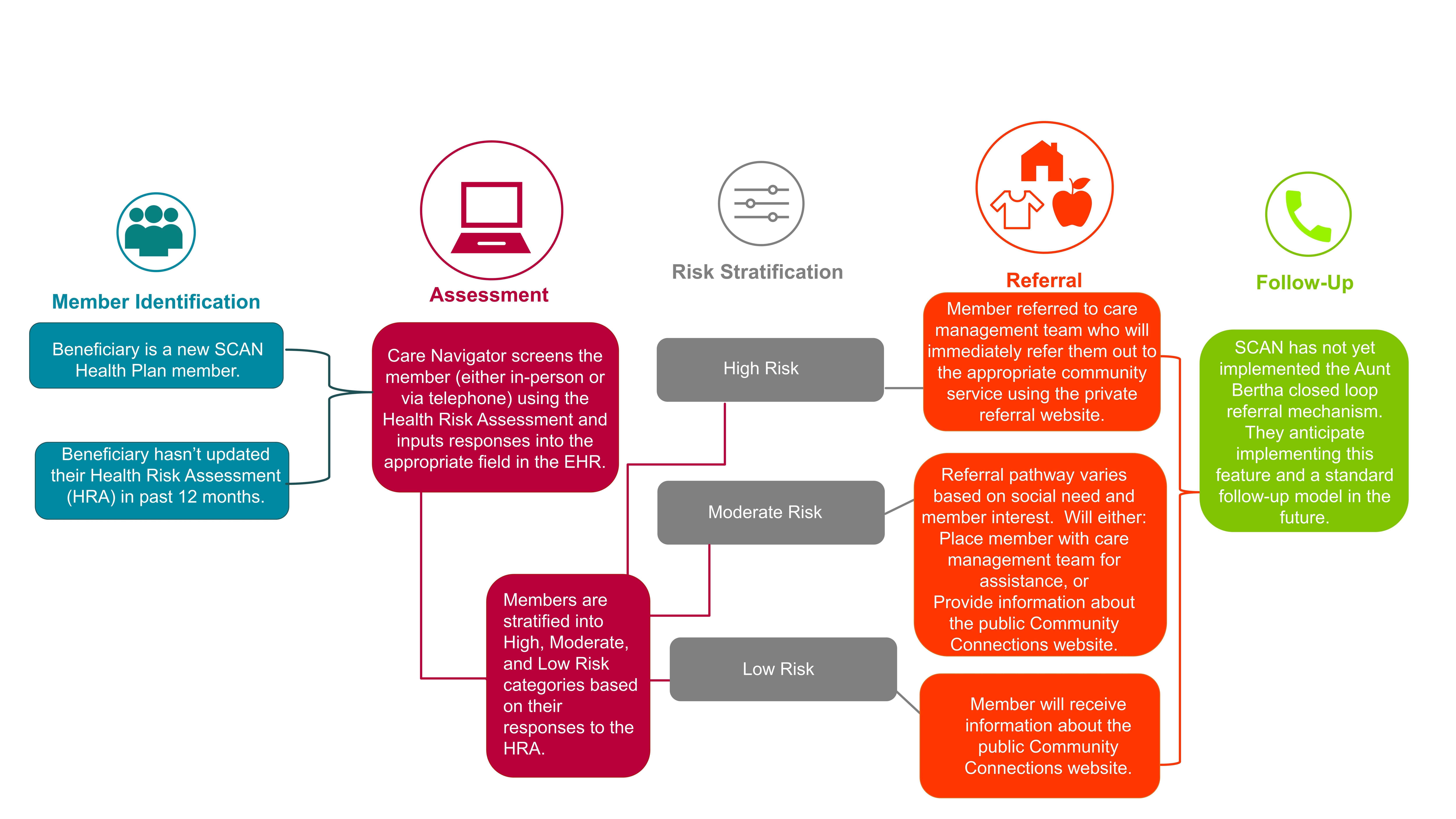
When developing a standardized approach for social needs screening and referrals, SCAN Health Plan wanted to avoid making major changes to existing workflows. It was also concerned about “survey fatigue,” since health plan members were already required to complete a variety of assessments. The health plan determined the least burdensome way to implement social needs screenings would be to incorporate additional social needs questions into an existing screening, the HRA.
The state of California requires all managed care plans to assess newly enrolled dual-eligible members for current health care risks using an HRA. Although the HRA is mainly focused on assessing patients’ medical needs, it does require screening for homelessness. It also requires that health plans have a protocol to refer members to housing services following a positive screen. Incorporating a few additional social needs questions into the HRA felt like a natural extension of SCAN’s existing work and a straightforward way to assess members’ social needs.
“The results from the HRA not only drive the type of programs we want to produce in the future, but they help inform how we navigate our existing programs: What do we need to focus on? What do we need to add to?”
—Project manager
The health plan initially piloted social needs screening with its SNP health assessment, and in 2016 it incorporated the social needs questions into the broader HRA for All. All health plan members are now assessed with the HRA upon enrollment and reassessed annually to determine how their social and medical needs change over time.
The HRA is conducted either in person or by phone and can take from 10 to 20 minutes to complete. Care navigators conduct the assessment and input member responses into SCAN’s care management software. Once the assessment is complete, members receive a care plan to address their unmet needs and may be enrolled in a care management program, based on their risk level and complexity of need.
Members are stratified into risk categories using SCAN’s electronic risk stratification algorithm. Based on the HRA, the referral processes vary depending on the trigger for referral. A high-risk member (e.g., someone with a positive screening for housing insecurity or elder abuse) will be referred immediately to the appropriate care management program and appropriate clinical and community resources. For moderate-risk members, the response varies based on the social need identified as well as the member’s interest in obtaining assistance. Members who are identified as low-risk will still typically receive educational materials and handouts about local service offerings.
Key Staff
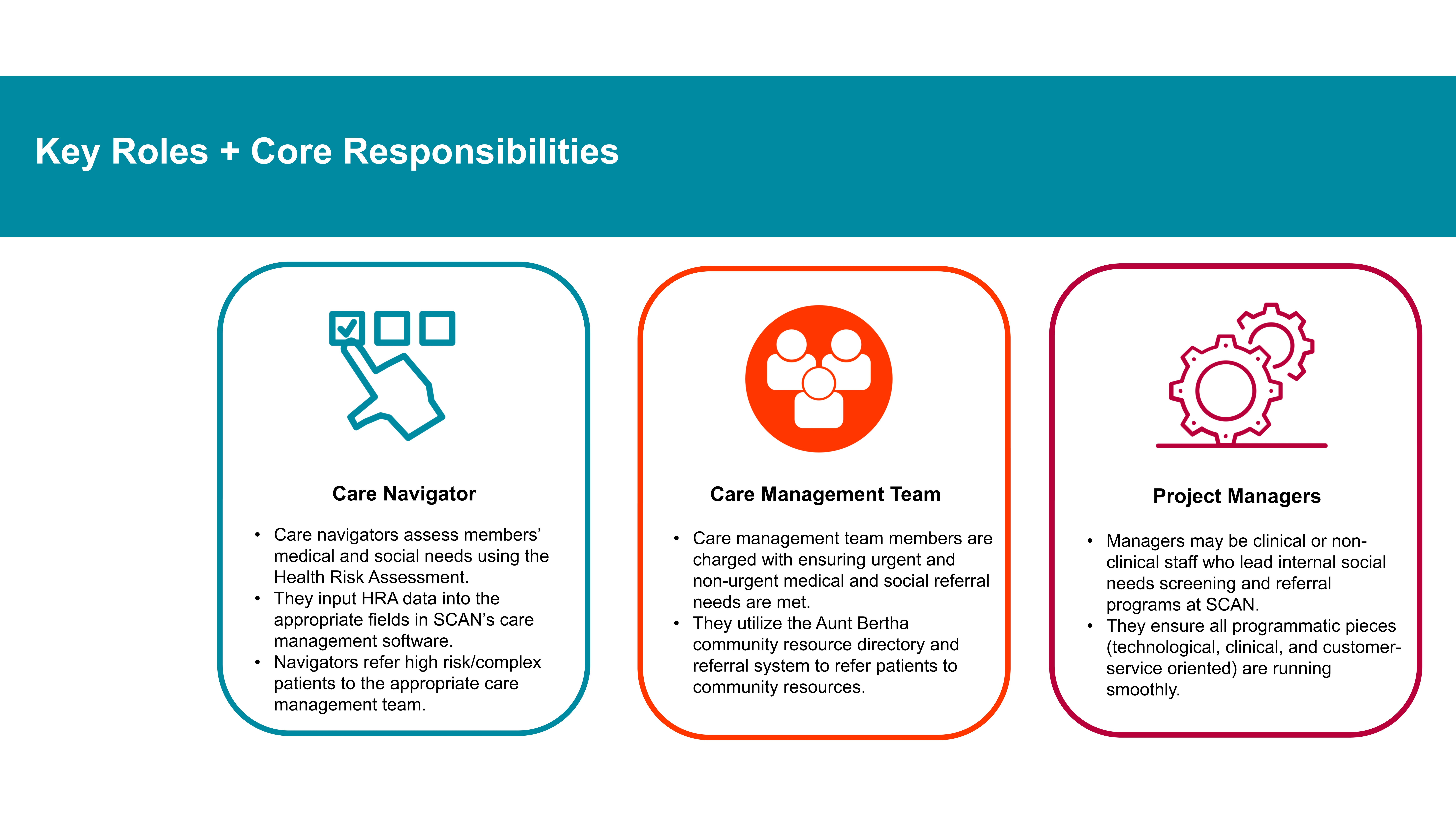
Numerous member-facing and operations staff work together to ensure SCAN’s social needs screening and referral model runs smoothly. The image below provides an overview of the major responsibilities associated with care navigators, complex care management, and project management roles.
Leveraging Technology to Facilitate Community Referrals
SCAN Health Plan has partnered with a vendor called Aunt Bertha to deploy an online community resource directory and referral system. Aunt Bertha is an interactive platform, allowing participation from members, staff, and organizations on a voluntary basis.
The resource directory and referral tool have been deployed in three specific ways:
- Public website: The member-facing website, Community Connections, allows members and their caregivers to search for resources on their own, as well as send referrals to family members or friends. Through the site, users are also able to save listings and develop a personal library of resources. The site is accessible through the SCAN website.
- Private referral website: The Aunt Bertha site allows SCAN staff to send referrals to members for programs and track the progress of the referral between the program and the member. Additionally, SCAN collects data on how the platform is being used, and this information is used to identify which programs have been searched the most, what category of services are most frequently sought, and what kind of organizations are seeing the highest number of referrals. SCAN has implemented single sign-on for staff, so that staff are automatically logged in when they access the SCAN network. Programs and community organizations have the ability to be as involved with Aunt Bertha as they would like — once their program/organization is listed on Aunt Bertha, they have the opportunity to “claim” their listing. Claiming a listing signifies that the program has verified the listing information and accuracy. Programs then have the opportunity to upload program forms, eligibility requirements, etc., to their listing. Furthermore, programs and community organizations have the option of closing the loop on referrals through Aunt Bertha by checking a box that indicates the referral is in progress, on hold, or complete.
- Anonymous staff website: SCAN is in the process of deploying a website for its own staff to use so they may anonymously conduct personal searches for themselves.
Each of these websites is linked to the same database of services but contains a different level of user anonymity and referral functionality. Over time, SCAN hopes to strengthen and expand its partnerships with community organizations to achieve:
- A higher number of “claimed” social service programs that are willing to receive and process electronic referrals
- A standard process for community organizations to close the loop once a member completes a referral
Results and Next Steps
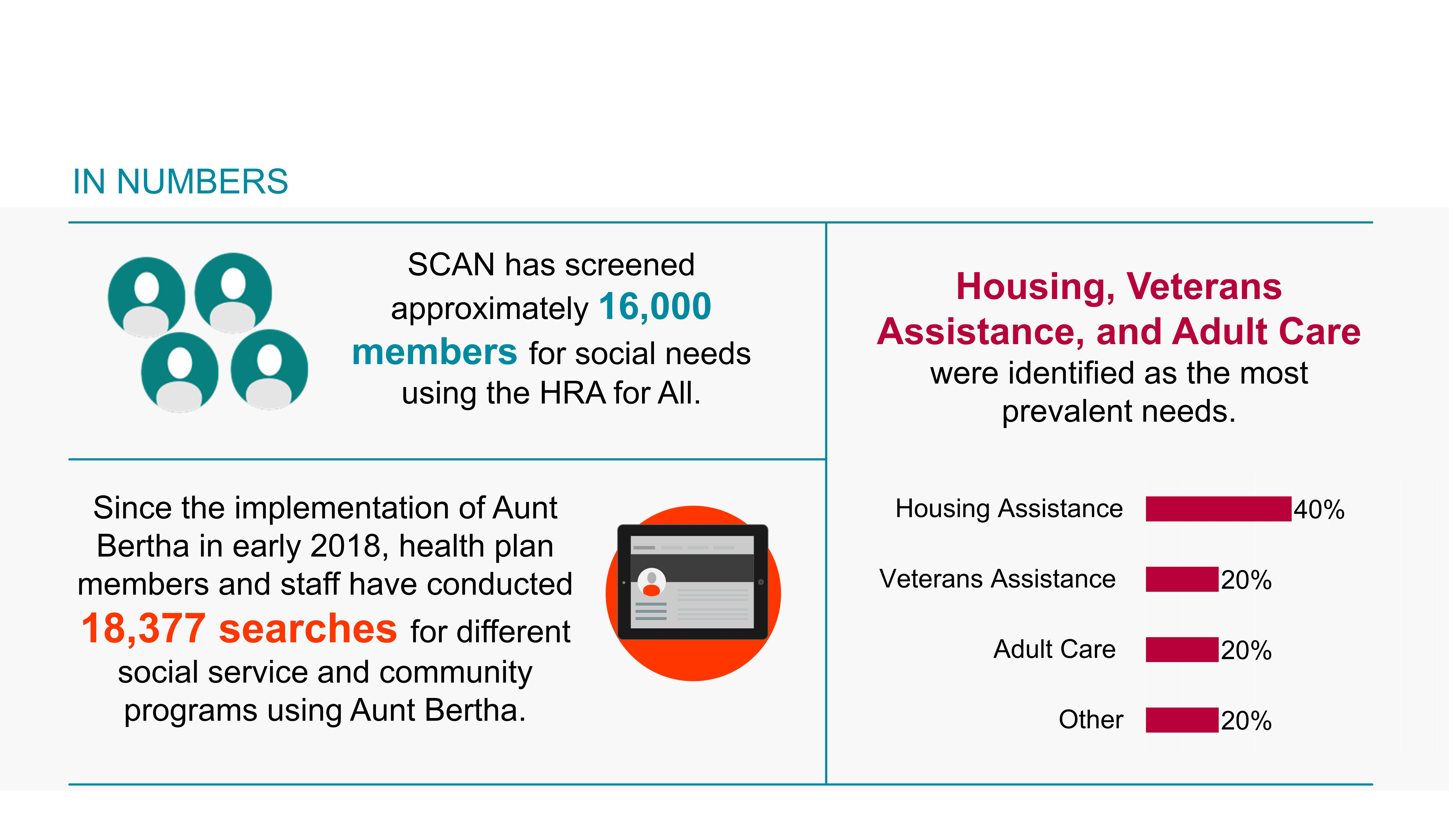
Since SCAN incorporated standardized social needs questions into the HRA for All in 2016, it has assessed approximately 16,000 members for social needs. In the past year, SCAN has used the Aunt Bertha community resource directory and referral system to conduct over 18,000 searches for members who need to access social and community services.
Next steps include implementing an internal Aunt Bertha website that staff may use to anonymously conduct personal searches for themselves and implementing the closed-loop referral feature. Although the health plan currently has the capacity to document closed-loop referrals through the Aunt Bertha system, there hasn’t been much uptake in this area. This is likely because community-based organizations need additional training to understand the importance of checking off the box to indicate when a referral is complete. SCAN hopes to strengthen and expand its relationships with community partners in the future so this feature may be effectively employed.
SCAN Health Plan’s Three Lessons for Social Needs Screening and Referrals
For those preparing to undertake a new social needs screening and referral project, the SCAN team shared the following lessons:
- Closed-loop referrals: Working with community-based organizations to close the loop on referrals using new software or a website can be time-intensive. Instead of implementing a community resource directory and closed-loop referral system simultaneously, consider a phased-in approach. Phase I may focus on securing buy-in and community resource directory uptake among internal staff, while Phase II may focus on engaging and providing trainings to the broader community.
- Asking the right questions: Identifying the social needs questions that can be tested, validated, and standardized is a major undertaking. The “correct” questions may vary by organization, based on how each balances different regulatory requirements with a person-centered approach.
- Philosophy of care and leadership buy-in: The process of implementing a standardized social needs screening and referral program for all members was made easier by the fact that leadership and staff had already bought into a patient-centered geriatric approach to care. The geriatric approach to care provides a holistic picture of a patient’s needs and includes a focus on managing psychological and social aspects of care in addition to caring for chronic diseases. It can be helpful to consider this approach even for populations that are not in the geriatric age category.
Notes
- SCAN Health Plan conducted this work on its own and without any funding or support from CIN or CHCF. ↩︎




