Overview
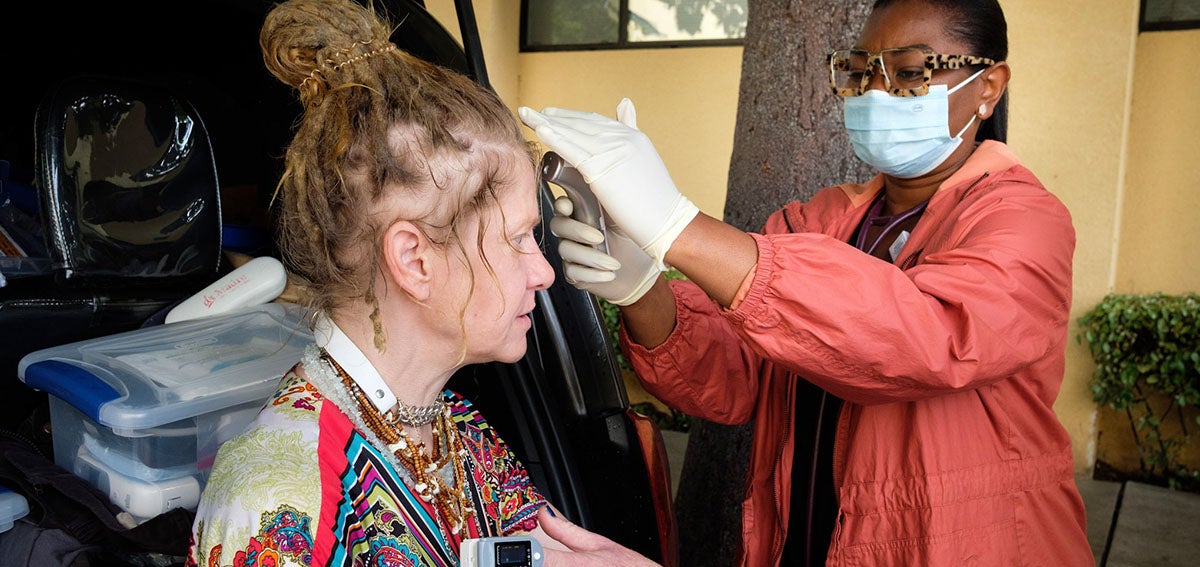
Homelessness and health are inextricably linked. People experiencing homelessness often face extensive physical and behavioral health needs. These needs can be further complicated by living in a car or on the streets.
Explore what part you and your organization can play so people are housed and healthy by learning more about:
The stories of people experiencing homelessness and what they tell us about how systems of care can better support them
- Medi-Cal reforms that support a whole-person approach to care and how they help address patients’ social needs
- Cross-sector partnerships, especially those between health care and homeless services providers, and how they streamline continuity of care
- Care delivery models that match patients’ needs, including those outside traditional clinical settings and how to scale them
- The stories of people experiencing homelessness and what they tell us about how systems of care can better support them
Medi-Cal and Homelessness
In January 2022, the California Department of Health Care Services launched CalAIM (California Advancing and Innovating Medi-Cal). This major reform has the potential to improve outcomes for the millions of people enrolled in Medi-Cal, including people experiencing homelessness. Of special note are two new programs.
Housing-Related Community Supports Covered in CalAIM
- Housing transition navigation services
- Housing deposits
- Housing tenancy and sustaining services
- Short-term posthospitalization housing
- Medical respite
- Sobering centers
- Day habilitation
Enhanced Care Management is a benefit available to people with complex needs, including those experiencing homelessness, to coordinate their care, which includes connecting them to treatment for any physical or mental health conditions and substance use disorder, and to social services.
Community Supports are a new set of 14 services not traditionally covered by Medi-Cal, including housing deposits and services to help people remain stably housed. Medi-Cal managed care plans have the option to offer these services to their members. (See box.)
Explore the resources below to learn more about implementing CalAIM reforms to meet the needs of people experiencing homelessness. You may also wish to visit CHCF’s CalAIM resource center filled with tools and resources explicitly for organizations implementing CalAIM programs.
Featured Resources
Housing and Homelessness Incentive Program
While most people experiencing homelessness are eligible or already enrolled in Medi-Cal, managed care plans have historically not been engaged in efforts to address homelessness. Through CalAIM that is beginning to change. While most Medi-Cal managed care plans are funding housing-related Community Supports, such as housing navigation and security deposits, many are not well connected to the larger homeless system of care. Building these connections can be difficult and costly but is crucial to the success of CalAIM’s commitment to improve outcomes for Californians experiencing homelessness.
The Housing and Homelessness Incentive Program (HHIP) offers Medi-Cal managed care plans the opportunity to earn incentive funds for building partnership with homeless systems of care. The program offers $1.3 billion of one-time funds available through the federal American Rescue Plan Act.
HHIP is a voluntary program, and managed care plans (MCPs) that choose to participate will work at the county level with local community stakeholders. MCPs must file an investment plan with the state which demonstrates a roadmap for achieving targets in collaboration with local partners. The state expects that MCPs will pass through the incentive funds to local partners by investing in work with local organizations that are leading housing- and homeless-related efforts.
Cross-Sector Partnerships
Homelessness is linked to factors such as physical health, mental health, economic opportunity, local housing supply and affordability, violence, racial inequity, and more. That’s why addressing homelessness requires collaboration across sectors, especially between health care and homeless services providers.
Envision
- Multiple systems working together effectively so people are housed and healthy
- No wrong door for getting help and services
- Strong cross-sector collaboration allowing for successful referrals to behavioral health treatment, housing and transportation support, food assistance, legal aid, support for older adults, and more
Cross-sector partnerships are created to improve coordination and make progress toward a shared goal. For example:
- A hospital system, managed care plan, and housing assistance provider may coordinate to assist patients at risk of homelessness after being discharged from the hospital.
- A health care provider and a homeless services provider may partner to deliver primary care at local homeless shelters and via mobile clinics.
Explore the resources below to learn how your organization can apply lessons from existing cross-sector partnerships.
Featured Resources
Street Medicine
People in California experiencing unsheltered homelessness face barriers accessing health care in traditional settings. They may not have transportation to primary care, preventive care, and nonurgent care facilities, or to pharmacies and specialists.
Street Medicine in California
- Street medicine is an important access point for people of color, with 25% of street medicine patients identifying as Black and 23% identifying as Latino/x.
- The majority of street medicine programs provide primary care services. More than two-thirds diagnose and treat mental health conditions and substance use disorders, with 60% providing medication-assisted therapy.
- Nearly all street medicine patients are insured, with at least 57% having Medicaid and 14% having Medicaid and Medicare.
Source: University of Southern California Keck School of Medicine, 2022.
Effective, responsive street medicine programs can play a role in addressing this challenge by bringing health care to where people are. Health care programs in these settings might include walking teams of providers, medical vans, and outdoor clinics.
Explore the resources below to understand existing street medicine models in California and the role you can play.
Featured Resources
Medical Respite
Medical respite — also referred to as recuperative care — programs provide room, board, and medical care coordination in a postacute care setting for people experiencing homelessness who are too ill or frail to recover from a physical illness or injury on the streets or in shelter, but who are not ill enough to be in a hospital.
Medical Respite in California
- Under CalAIM, managed care plans can offer recuperative care (PDF) as a Community Support.
- Across California, no two medical respite programs operate the same way. Each can be designed to meet community and partner needs.
- The Illumination Foundation, based in Orange County, runs one of California’s largest medical respite programs. Over 18 months, this program saved more than $17 million in medical costs for 1,200 CalOptima patients.
These programs are emerging as an important intervention for people experiencing homelessness following a hospital stay or outpatient surgery that requires a stable setting for recovery.
Effective recuperative care reduces hospital admissions and dependence on emergency rooms. It also provides more opportunities for people experiencing homelessness to get connected with support services and transitional housing.
Explore the resources below to learn more about how medical respite works and how to grow these programs.
Featured Resources
Watch the video
Sobering Centers
Sobering centers are short-term care facilities that allow people who are intoxicated to safely recover from the effects of alcohol or other drugs.
Open 24 hours, these centers can reduce drug overdose injuries and deaths within the community and serve as an effective alternative (PDF) to the emergency medical system.
Sobering centers can be a bridge to housing and health when they include:
- Referrals to community resources providing longer-term care for people with substance use and mental health issues
- Homelessness services like housing navigation, case management, and referrals to transitional housing
For people experiencing homelessness while living with substance use disorder, sobering centers provide both critical short-term care as well as an entry point for more comprehensive, long-term, and preventive care. Under CalAIM, managed care plans can offer sobering centers (PDF) as a Community Support.
Explore the resources below to learn how sobering centers can be a bridge to housing and health and how this model can be replicated in your region.
Data Exchange
To provide effective help to people experiencing homelessness, different systems and partners need to be able to share data seamlessly. Data exchange enables better coordination between sectors to meet patient or client needs. Different cross-sector partnerships have found creative solutions to common data sharing challenges, such as privacy issues and interoperability.