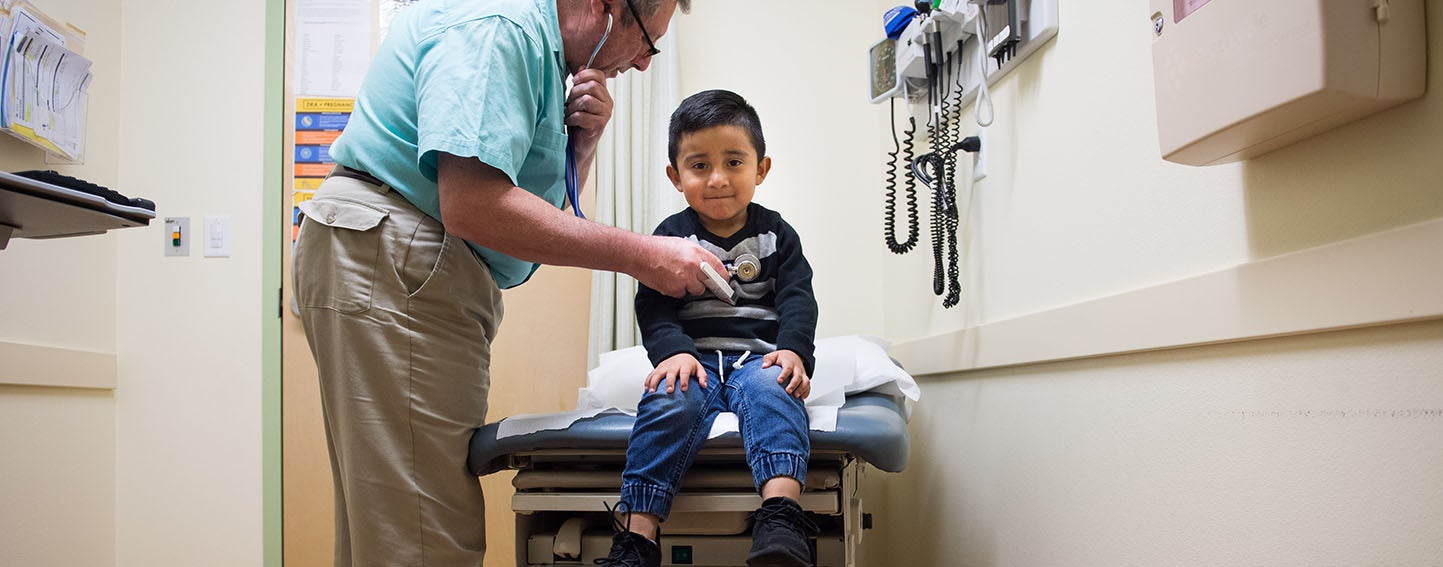
More than 10 million Californians — mostly children, their parents and caretakers, people with disabilities, and adults typically in low-wage jobs — get their health care through a managed care plan in Medi-Cal, the state’s Medicaid program. They rely on their Medi-Cal managed care plan to provide timely access and high-quality care. This includes services such as regular well-child visits and prenatal care, health screenings to catch and treat life-threatening diseases early, and proper treatment of chronic conditions so they don’t lead to disability or premature death.
Unfortunately, data collected by the state have long shown that access to care and the quality of care provided to Medi-Cal managed care enrollees varies widely across regions and even among plans within the same county. In addition, two recent state audits highlight problems both for children statewide and for populations in rural areas.
Two New Studies
Today CHCF released two studies that add to our understanding of the quality of Medi-Cal managed care and offer ideas for improvement. Researchers at the University of California, San Francisco, showed that from 2009 to 2018, the quality of care for Medi-Cal managed care enrollees, on average, stayed the same or declined for over half of the quality measures monitored by state health care officials. Particularly disappointing was the fact that quality declined or stayed the same for six of the nine measures related to care for children, including access to primary care and well-child visits. Simply put, we just haven’t seen the type of quality improvement over the last decade that we would expect from a program as important to our state as Medi-Cal.
The study also shows that Medi-Cal enrollees in nonprofit or public managed care plans received, on average, better quality care than those in for-profit plans. Those living in counties with a County Organized Health System received, on average, better quality care than those in counties with competing managed care plans. (For more background on the types of plans and models in Medi-Cal managed care, see this resource from CHCF’s Medi-Cal Explained series.) In other words, some enrollees are more likely than others to get the care they need when they need it simply because of where they live or the health plan they are enrolled in. To understand trends in quality of care in your area, see these local snapshots.
The good news is that major improvements in quality are possible. A companion study by Chapman Consulting examines a few managed care plans that have increased their scores on several quality measures during the same time frame. The study points to several interconnected strategies that are key to quality improvement, including real-time data exchange, collaboration with providers at the point of service, and targeted financial incentives, among others. This information should inform Medi-Cal’s efforts to expand and accelerate quality improvement in managed care.
Five Ways for California to Improve Quality of Care
State officials should act swiftly to ensure that all enrollees, regardless of where they live or which plan they are enrolled in, have timely access to high-quality care. Some of these actions can be taken immediately. Others could be pursued as part of a bold new vision that guides both the upcoming planning process for the renewal of two federal Medicaid waivers, as well as the contract renewal process for commercial Medi-Cal managed care plans that begins next year. These waivers and this reprocurement are infrequent and important opportunities to reshape the program. Here are five important steps California should take:
1. Establish clear, measurable quality goals for the Medi-Cal managed care program and for individual plans, with a focus on continuous improvement.
The Department of Health Care Services (DHCS), which administers Medi-Cal, recently signaled that it was raising expectations by increasing plans’ minimum performance level (MPL) on quality measures from the 25th percentile nationally to the 50th percentile. While the intent is laudable, this approach falls short.
It fails to set the expectation that managed care plans should continue to improve quality even when their scores are at or just above the 50th percentile. It also doesn’t recognize that it is easier for managed care plans in some counties to achieve high-quality care than plans in other counties because of differences in the underlying workforce, capabilities of safety-net providers, or other factors. Kaiser Permanente, for example, currently gets to control who enrolls, an advantage no other Medi-Cal managed care plan has.
Finally, it rewards some gains more than others. With the MPL set at the 50th percentile, a plan would be better off improving its score on a quality measure from the 49th to the 51st percentile than it would be for improving its score on another measure from the 25th to the 35th percentile. It would be better to establish plan-specific targets for continuous quality improvement. State officials should also “walk the talk” by setting specific, measurable, program-wide improvement targets for Medi-Cal.
2. Pay plans based on quality.
With his value-based payment initiative, Governor Gavin Newsom has shown he understands how important it is to pay health care providers based on quality and outcomes, not just on the volume of services they provide. It’s time to extend this principle to the way California pays Medi-Cal managed care plans and use financial incentives to drive quality improvement, as I’ve written about previously. Several states have already paved the way. One model would allow plans to share in the savings they produce when higher-quality care leads to savings such as reduced hospital admissions as long as plans meet defined quality benchmarks.
3. Eliminate data blind spots related to disparities and delegation.
Research, including this DHCS report on disparities in 2015 (PDF), shows that quality of care in Medi-Cal varies widely by race and ethnicity. We can’t improve what we don’t measure, so DHCS should be monitoring and regularly reporting on access and quality in Medi-Cal managed care by race and ethnicity — and making this data easily accessible for others to study. This will enable DHCS to identify challenges, learn from successes, and focus improvement efforts. Similarly, many managed care plans subcontract with other plans or risk-bearing provider groups but do not report quality scores separately for these subcontracted partners. For example, members of Los Angeles County’s L.A. Care plan can get their care directly through L.A. Care or choose one of three plan partners: Anthem Blue Cross, Blue Shield Promise Health Plan, or Kaiser Permanente. These managed care plans and medical groups should be required to report the same access and quality data as plans that contract directly with DHCS, so state officials can assess their performance and enrollees can make informed choices.
4. Consider restructuring the Medi-Cal managed care system.
Enrollment in Medi-Cal managed care has more than doubled since 2013, yet there have not been significant changes to the underlying structure of the program since it was established over 20 years ago. The new studies suggest it’s time to reconsider the different models of managed care and the role of competition. For example, given their track record on quality compared to public and nonprofit plans, what role should for-profit plans have in Medi-Cal managed care? Similarly, should the state look to encourage existing or new public plans to serve in areas where there are currently only commercial plans?
Two forthcoming papers from CHCF, which provide deeper analysis of quality and access specifically under the Geographic Managed Care Model and the Regional Model of managed care, will offer further insights into ways DHCS might want to structure the system differently. The papers will be published in October.
5. Continue to invest in delivery system transformation and in the health care workforce, especially in rural areas.
Many of the problems documented in these studies didn’t start with managed care and can’t be solved by managed care plans alone. The experiences of County Organized Health Systems that serve enrollees in multiple counties highlight the fact that some areas are more difficult to serve than others, even when a plan has strong leadership and is rooted and investing in its communities. Managed care plans serving rural areas have far fewer health care providers and less robust health care infrastructure available. This limits their ability to provide timely access and to deliver high-quality care.
Recognizing that this will be a decades-long effort requiring political will and resources, the state must launch long-term investments and partnerships to build the health care workforce, especially in rural areas. The 2019–20 state budget, which provides hundreds of millions of dollars in state funding to ease mental health workforce shortages and low rates of physician participation in Medi-Cal, was a significant first step.
California should also continue to invest in innovative programs that provide financial incentives and support to transform public hospitals and other safety-net providers and to reorient them to provide greater value. For Federally Qualified Health Centers, which account for a disproportionately large share of primary care for Medi-Cal managed care enrollees, value-based payment should be a priority.
A Healthy California for All
Over the past six years, California has dramatically expanded Medi-Cal and halved the uninsured rate, improving access to care for millions of Californians who otherwise would be uninsured. It’s a remarkable achievement we should all be proud of. Yet there is more work to be done to fulfill the promise of this coverage. Working together, we can heed Governor Newsom’s call to build a “California for All” by creating a system where all Medi-Cal managed care enrollees — no matter where they live or which health plan serves them — get the timely, high-quality care they need to thrive.
Authors & Contributors


Jessica Brandi Lifland
Jessica Brandi Lifland is a freelance photographer, instructor of journalism at City College of San Francisco, and mother. Her work with publications and nonprofits such as Operation Smile, Tostan, and the California Health Care Foundation has taken her all over the world, including West Africa, the Middle East, Kosovo, Burma, Haiti, and South America.
For two decades she has been photographing the National Cowboy Poetry Gathering and has been working on a long-term project documenting the lives of the cowboy poets of the American West in affiliation with the Western Folklife Center. She plans to make her project into a book.





