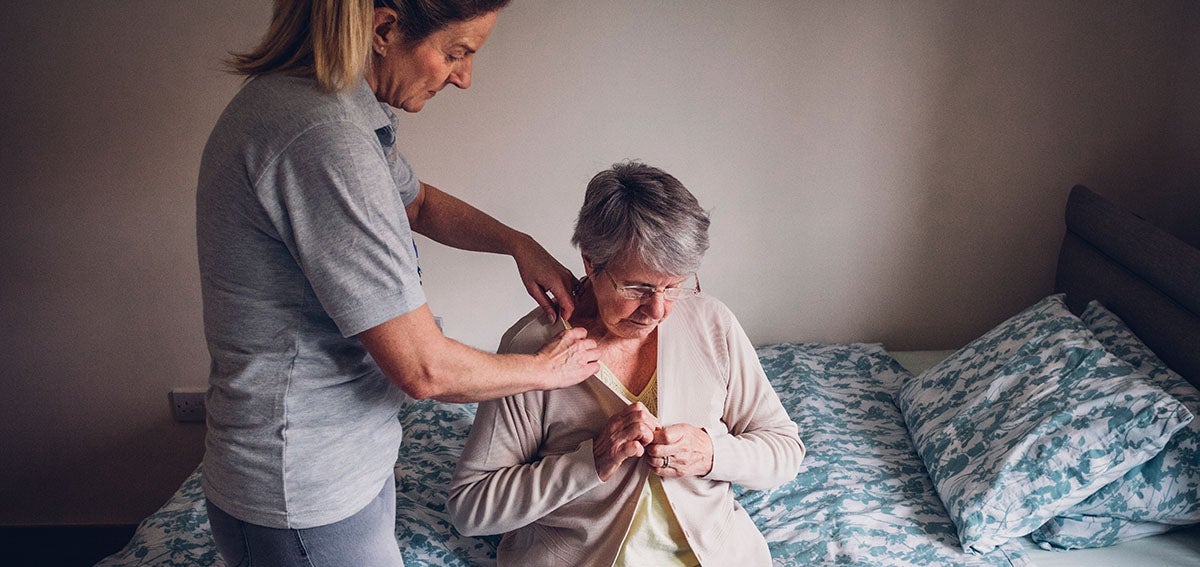
By 2030, the number of Californians age 60 and over will reach 10.8 million — almost double what it was a dozen years ago — and CHCF’s 2023 California Health Policy Survey has striking findings that highlight some of the health care challenges the state’s older adults face.
The poll shows that Californians are acutely aware, at a personal level, of our health systems’ weaknesses serving older adults and others with chronic illnesses or disabilities. Sixteen percent of Californians say they are providing living assistance to a family member or close friend, including help such as bathing, cooking, housecleaning, or paying bills. Californians with incomes below 200% of the federal poverty level are more than twice as likely as those with higher incomes to be providing this support (29% compared to 12%). Overall, less than one-quarter (23%) of these caregivers are paid to provide this essential care.
The poll also reports that 44% of Californians say they are “not too” or “not at all” confident that they will have the financial resources to pay for home-based support that might be needed by their family members or themselves as they get older. That concern is more pronounced among Black Californians (52%) and people with low incomes (56%).
According to the poll, nearly three-fourths of Californians (72%) want to live at home if they ever need ongoing living assistance. More than one-third (35%) of those who needed home-based support in the last year could not get it: They couldn’t afford it, didn’t know where to find it, or the help they needed wasn’t available in their area.
These are painful reflections of today’s fragmented health care system. For the most part, Medicare doesn’t cover these services, and the patchwork of state and community-based programs that serve older adults and people with disabilities have often been hard to find and difficult to navigate. People are deeply concerned about this system colliding with major demographic shifts taking shape. There will be millions more older Californians in the future than we have today, many will need help at home, and fewer younger people will be in the workforce to provide that help.
While health and social services programs have struggled to meet the complex needs of older people in the past, it’s clear that state leaders are committing time and resources to address many of the very issues that seniors and advocates for older adults worry about.
Dozens of Strategies to Help Seniors
This, after all, is the purpose of the state’s first-ever Master Plan for Aging (MPA), released in 2021, which includes dozens of strategies for developing more affordable housing options for people as they age, plugging gaps in the health system encountered by seniors, and preventing the isolation of older adults. It is no small thing that the Newsom administration, the California Department of Aging, the Department of Health Care Services, and myriad other state agencies and departments are working to implement scores of initiatives under the Master Plan. (Check out the state’s progress on the regularly updated MPA Implementation Tracker.)
The state’s CalAIM initiative also includes multiple new programs that will significantly expand the support system for older Medi-Cal enrollees, and make long-term services and supports more consistent statewide. One of the most promising is a new program called Community Supports, which provides managed care plans with a menu of 14 reimbursable services they can offer enrollees as cost-effective alternatives to traditional medical care. Several of them are intended to help older adults remain living independently in their homes and communities. These include:
- Personal care and homemaker services. Assistance with a variety of daily tasks, including bathing, dressing, toileting, moving about, and eating, as well as grocery shopping and money management
- Medically tailored meals. Delivered meals to support proper nutrition and manage chronic disease
- Home modifications. Physical adaptations to a home, including installation of grab bars, stair lifts, and wheelchair ramps, to enable older adults or people with disabilities to enjoy greater independence
- Caregiver respite. Short-term relief for in-home caregivers
- Nursing facility transition to assisted living. Coverage of the one-time expense of facilitating a transition to an assisted living community from a home or a nursing facility
- Nursing facility transition to home. Coverage of up to $7,500 in one-time expenses to help nursing home residents find housing in the community, including costs for transportation and moving
Older Medi-Cal enrollees can also be supported by another CalAIM program, Enhanced Care Management (ECM), a recently implemented benefit that connects people with complex health needs to a single care manager who can help coordinate care and services. Starting last month, the state requires that ECM services be provided to adults who are at risk of institutionalization and who are eligible for long-term care, and to adult residents of nursing facilities who are moving back to the community.
As these programs get underway, there are already promising stories of the impact they are having, including helping people move out of nursing homes and into residential settings.
The success of these CalAIM strategies will depend on the participation and leadership of managed care plans, as well as the willingness of plans and community-based organizations to work together to provide the services that aging Californians need. Despite the legitimate worries Californians have about how the health system cares for people who need help at home, the good news is that both are starting to happen. It gives me hope that California can do what’s needed to care for our growing population of older adults.
Authors & Contributors





