
Behavioral Health
The burden of untreated behavioral health conditions — encompassing mental health and substance use disorders — is both a major public health problem and a delivery system challenge. CHCF works to improve systems of behavioral health care and to focus on integrating mental health, substance use, and physical health services to achieve the best outcomes for Californians with low incomes.

Facts and Data
Our research provides essential information on California’s health care landscape to drive improvement. We collect, analyze, and share timely data to inform policymaking, identify disparities, and support evidence-based solutions for a more equitable health system.

Health Care Costs/Affordability
Rising health care costs remain a major challenge in California and across the nation. CHCF’s work sheds light on trends in state and national health care spending, as well as on the affordability of health care for consumers, to spur dialogue and action toward policy solutions.

Health Equity
All Californians should have the opportunity to achieve their fullest potential for health. CHCF is working with a wide range of partners to remove structural barriers to care and build a just and equitable health care system that is designed to redress, not perpetuate, the inequities that too many of our fellow Californians face.
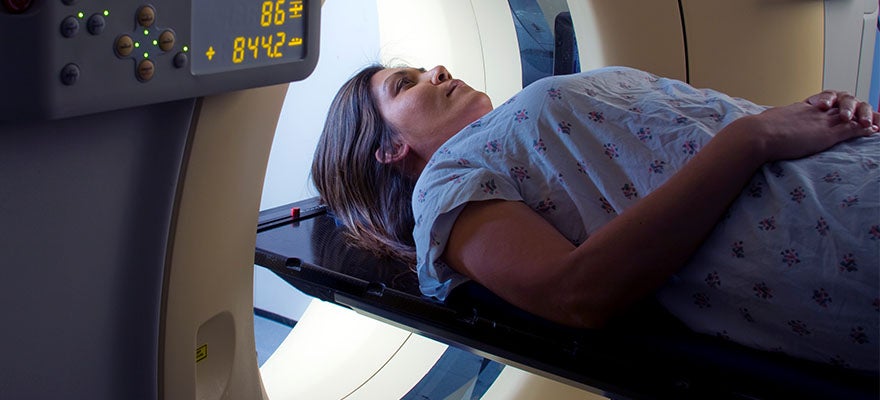
Health Insurance Coverage
During the COVID-19 pandemic the percentage of Californians with insurance has hit an all-time high. However, much work remains to ensure that all Californians can get and stay covered. CHCF produces data and analyses to inform efforts to protect coverage gains and further expand coverage so that all Californians can get the health care they need.

Health Workforce
Over the next decade, California faces a number of health workforce challenges, including a population that is growing, aging, and becoming more diverse. To meet these and other challenges, California must develop a modern health workforce that delivers smarter, more affordable care. That will require a new generation of health professionals with roles, skills, and workflows that match our latest understanding of how best to deliver high-quality, high-value care.

Homelessness
On any given day, more than 150,000 people experience homelessness in California. Being homeless is dangerous to your health: People who live on the streets die an average 20 years earlier than people who are housed. CHCF has launched work to improve the delivery of health and social services to people experiencing homelessness, with the goal of promoting care that is responsive, person-centered, and focuses on the patient’s emotional, physical, and psychological needs.
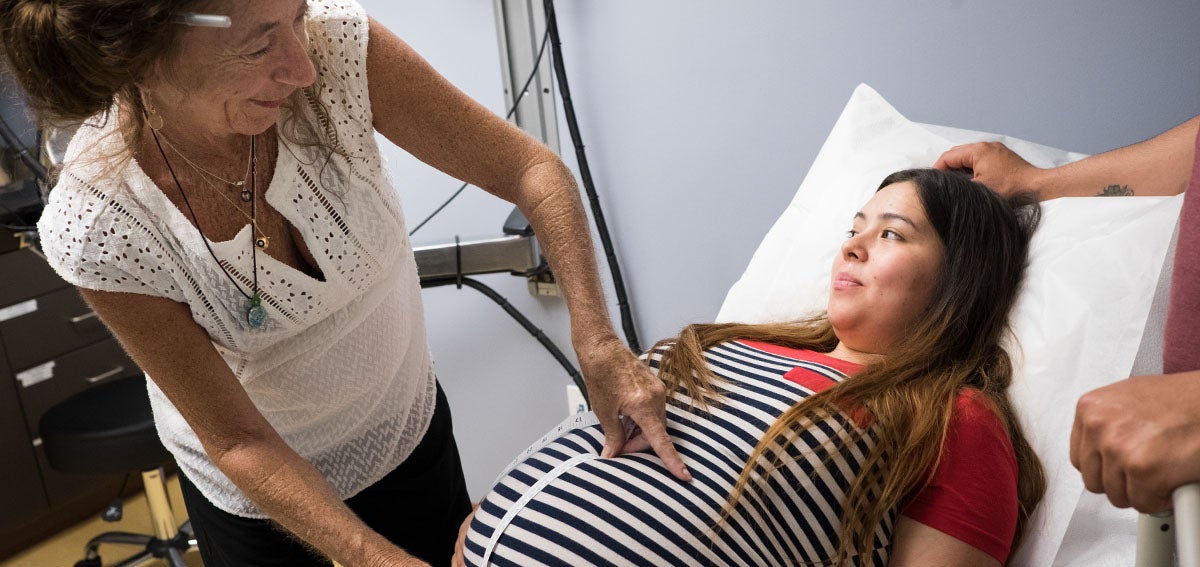
Maternal Health
Giving birth is the primary reason for hospitalizations in the US and California. Annually, 500,000 babies are born in the state, with half paid for by Medi-Cal. There are significant, unwarranted variations in maternity care quality, alarming disparities, and wasted resources. CHCF aims to improve quality and lower the costs of maternity care in California, especially for birthing people with low incomes, by ensuring appropriate care and reducing disparities in outcomes.

Medi-Cal
Medi-Cal is the state’s health insurance program for Californians with low incomes, including over 40% of all children, half of those with disabilities, over a million seniors, and one in five workers. CHCF reports provide data and analysis on how well Medi-Cal is serving Californians.

Older Adults
Too many older adults with complex health issues face multiple obstacles to getting the care and support they need. There are nearly three million Californians over age 50 who struggle to make ends meet while also facing significant health challenges. These adults, who get their care through Medi-Cal and, in some instances, Medicare, describe themselves as being in fair or poor health, and two-thirds report a disability due to a physical, mental, or emotional condition.

Primary Care
Our work in primary care strengthens the foundation of California’s health system. We support initiatives to expand access, enhance quality, address workforce shortages, and promote team-based care models that deliver comprehensive, culturally responsive services.

Technology and Innovation
From ending the opioid crisis to making care affordable for all, solving health care’s most intractable challenges will require innovative solutions. Through direct investments, grants, and partnerships, CHCF helps innovations succeed and scale in the safety net.
