View the Report
Jump to All Downloads & LinksIntegrating behavioral health into primary care is an important way to increase access to effective behavioral health treatment while maximizing the capacity of our very limited behavioral health workforce. There are many approaches to integration, but the Collaborative Care Model (CoCM) has the most robust evidence base, especially for anxiety and depression. CoCM adds two new members with behavioral health expertise to the primary care team, expanding the team’s capability to identify and treat people with common behavioral conditions.
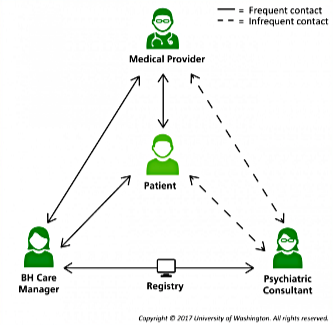
(“Team Structure,” Univ. of Washington)
Despite an evidence base including more than 80 randomized controlled trials, CoCM has struggled to scale nationally. A key barrier has been reimbursement — many of the activities required by CoCM do not neatly map to traditional billing codes. Recognizing both this barrier and the clinical potential of CoCM, the Centers for Medicare & Medicaid Services (CMS) introduced unique CoCM billing codes in 2016.
CMS established requirements for providers billing the CoCM codes for Medicare enrollees. Other payers, including state Medicaid authorities and managed care plans, can choose either to copy the CMS guidance or to revise the guidance — or decline to implement the codes altogether.
Nineteen state Medicaid agencies are currently covering CoCM, including California, which introduced CoCM as a benefit in January 2021.
These two documents are available as downloads further below:
Cracking the Codes: State Medicaid Approaches to Reimbursing Psychiatric Collaborative Care is a detailed report published in September 2020 that examines the state-by-state differences in how Medicaid agencies are choosing to implement and reimburse the CoCM codes, and summarizes the lessons and best practices gleaned to date.
An accompanying short fact sheet, Psychiatric Collaborative Care Management Benefit in Medi-Cal outlines California’s implementation choices. It summarizes the benefit, outlines the new billing codes, and provides an overview of how providers working in different settings can be reimbursed.





