View the Report
Jump to All Downloads & LinksGet These Charts
Our charts are available to use in your presentations and publications. Download a zipped file of all of the charts from this report, and review our Terms of Use.
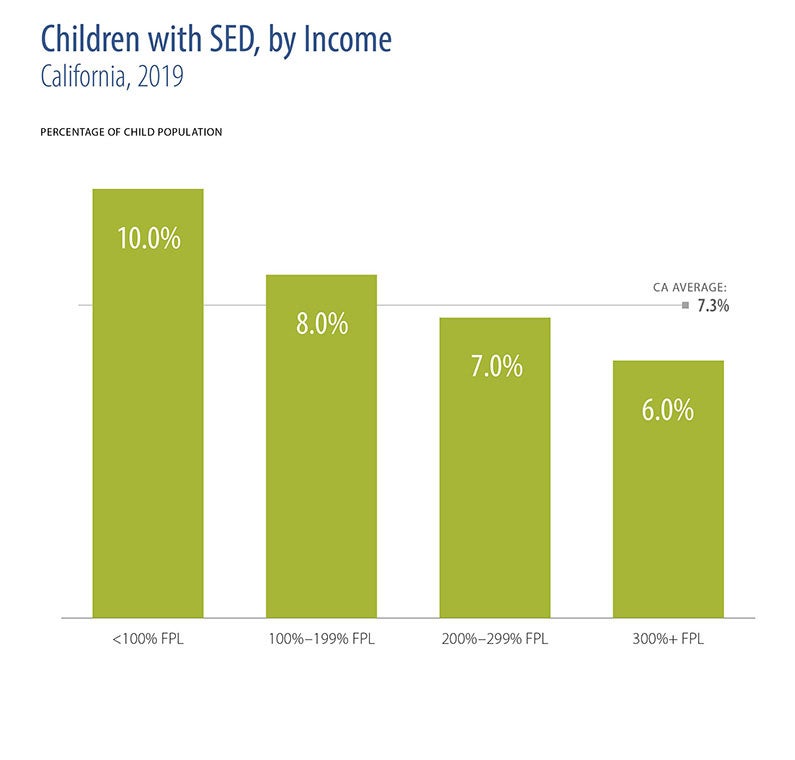
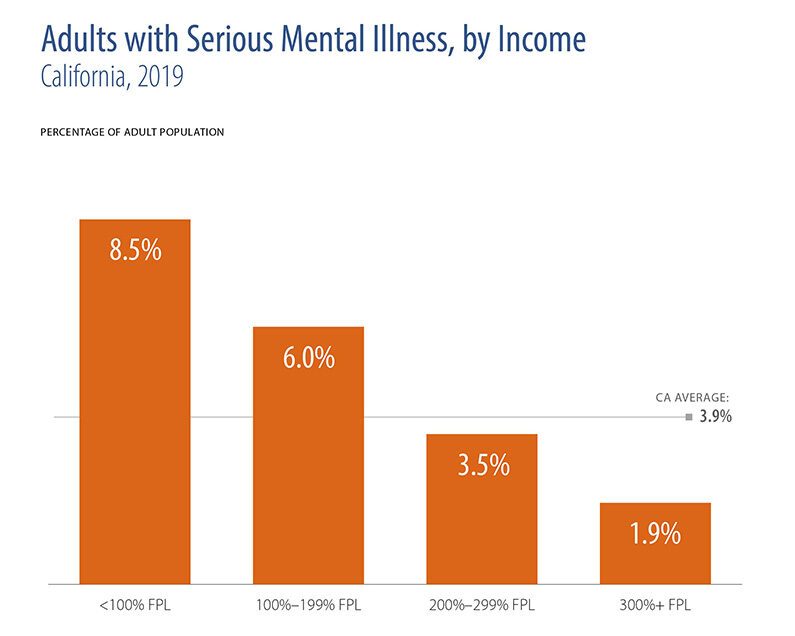
Mental illnesses are among the most common health conditions faced by Californians: Nearly 1 in 7 California adults experiences a mental illness, and one in 26 has a serious mental illness that makes it difficult to carry out daily activities. 1 in 14 children has an emotional disturbance that limits functioning in family, school, or community activities.
A number of positive changes have helped strengthen California’s mental health system. These changes include federal and state laws mandating parity in coverage of mental and physical illness, and the expansion of Medi-Cal eligibility and scope of mental health services under the Affordable Care Act. In addition, there have been numerous public and private efforts to expand access to care, encourage better integration of physical and mental health care, and reduce stigma. Nonetheless, a majority of Californians who need it fail to receive needed care.
Using the most recent data available, Mental Health in California: Waiting for Care provides an overview of mental health statewide: disease prevalence, suicide rates, supply and use of treatment providers, and mental health in the criminal justice system. The report also highlights available data on quality of care and mental health care spending.
Selected Findings
This slideshow displays highlights from the full report, which is available for download below.
Key findings include:
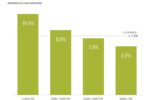
- The prevalence of serious mental illness varied by income, with much higher rates of mental illness for both children and adults in families with incomes below 100% of the federal poverty level.
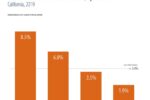
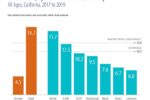
- Rates of serious psychological distress reported by California adolescents and adults increased between 2016 and 2019.
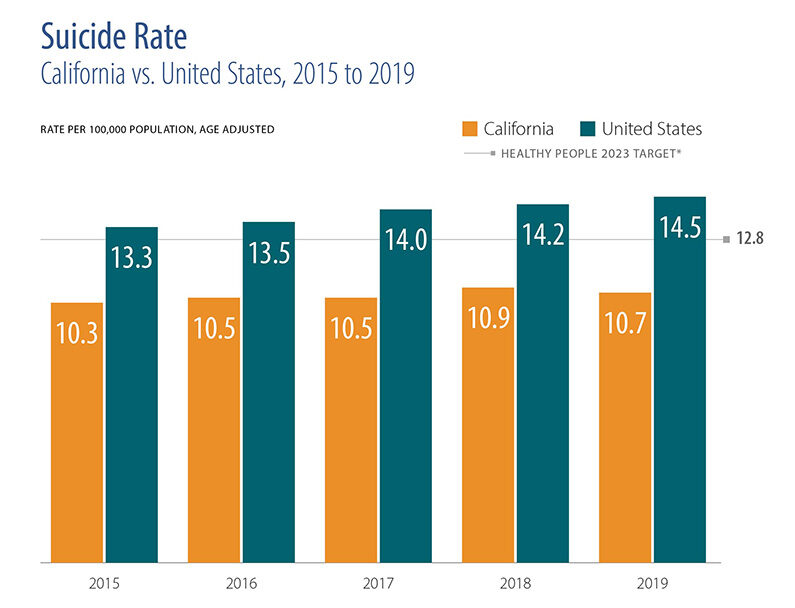
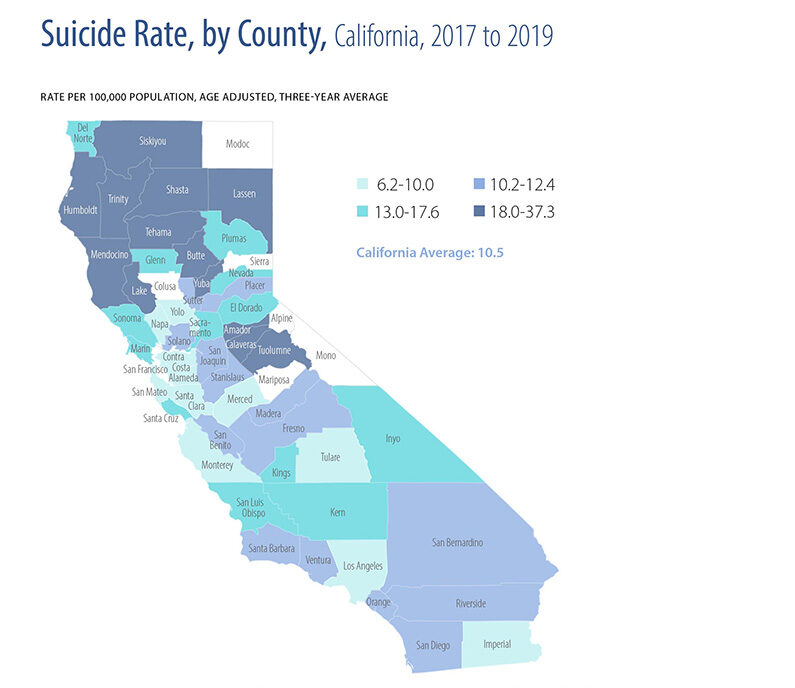
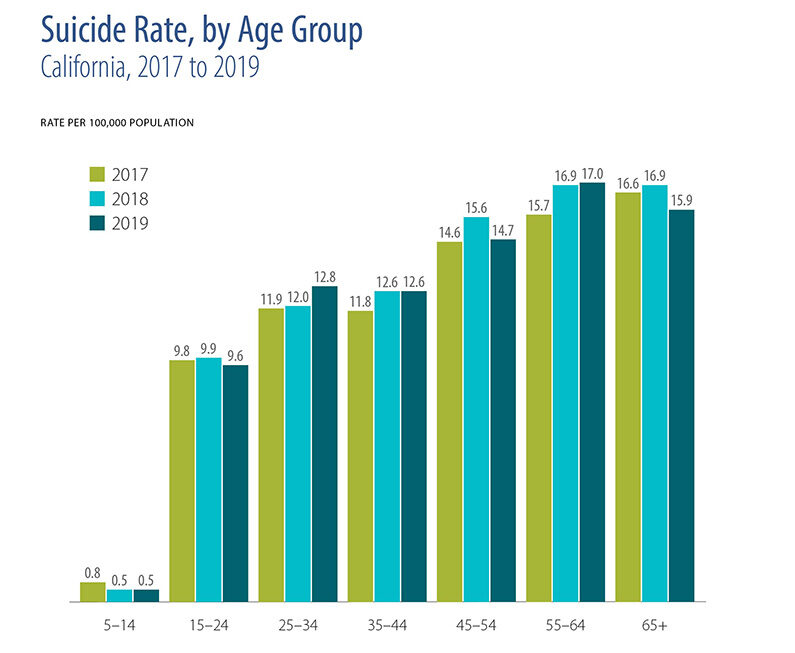
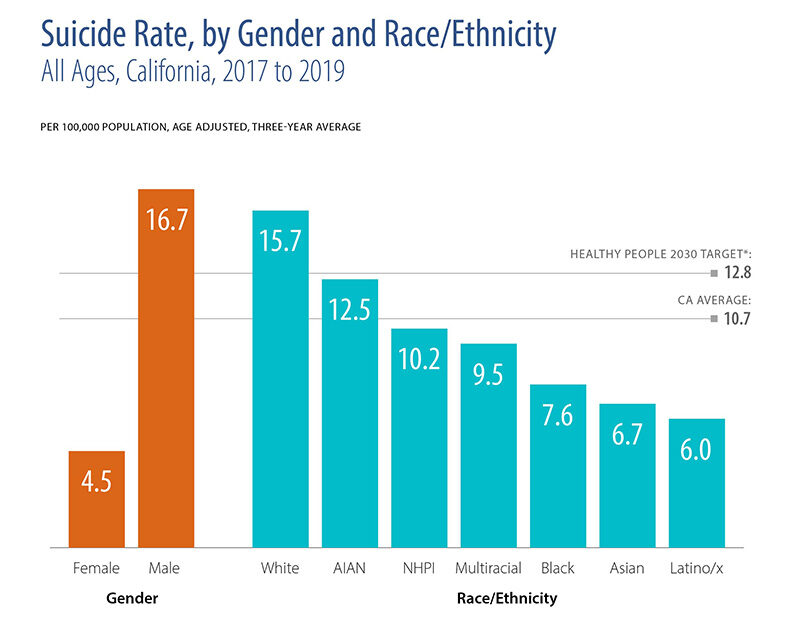
- California’s rate of suicide was below both the national rate and the Healthy People 2030 target, although rates varied within the state by gender, race/ethnicity, and county.
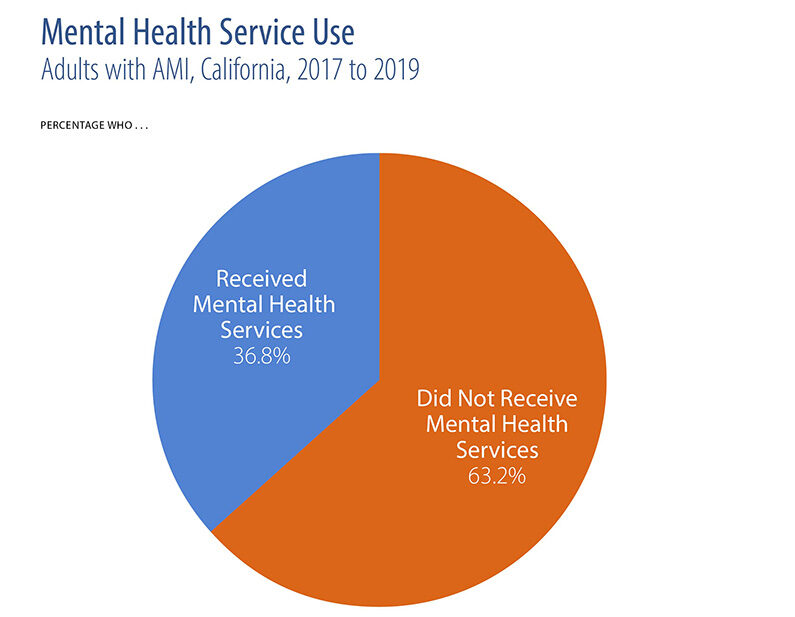
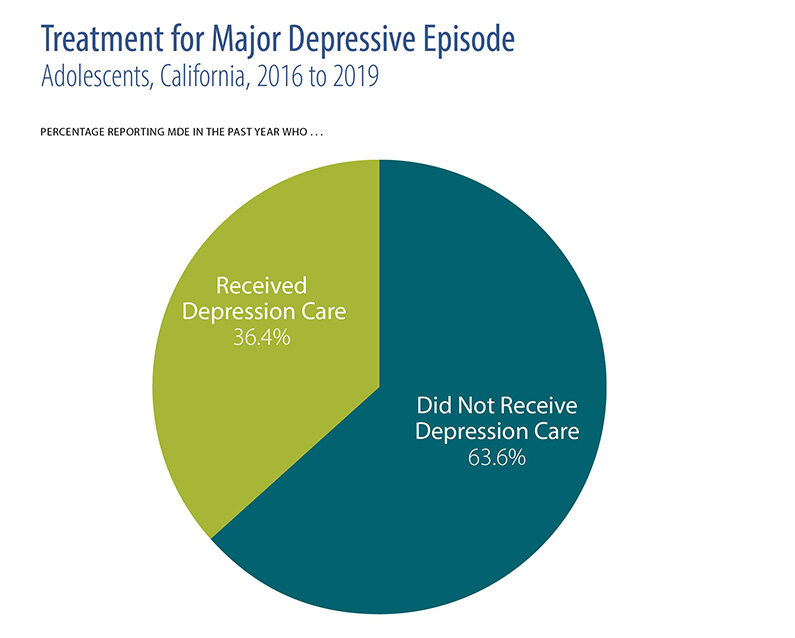
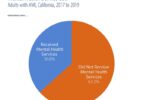
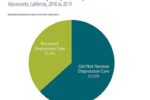
- Close to two-thirds of adults with a mental illness and two-thirds of adolescents with major depressive episodes did not get treatment.
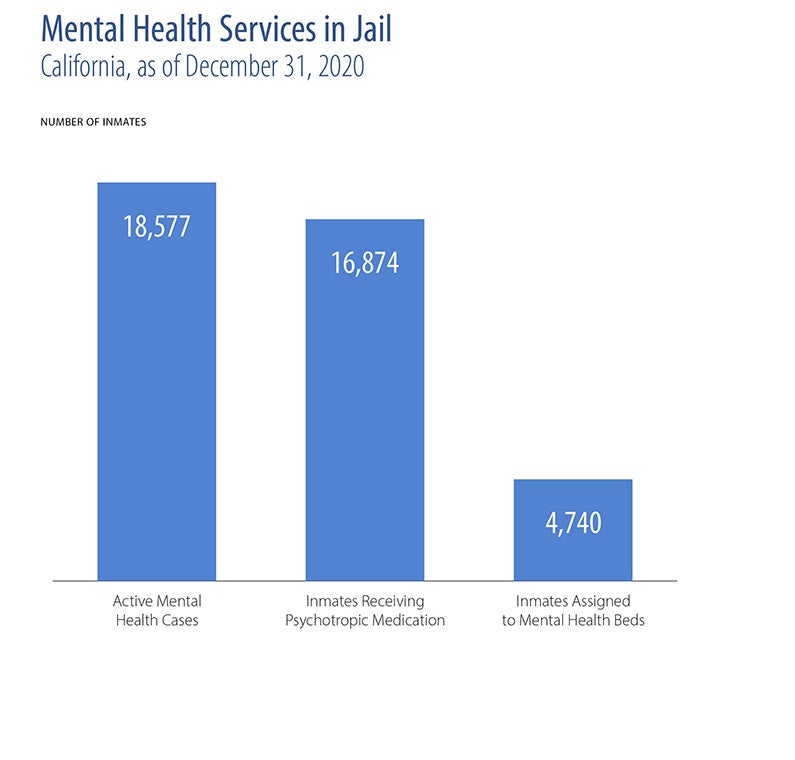
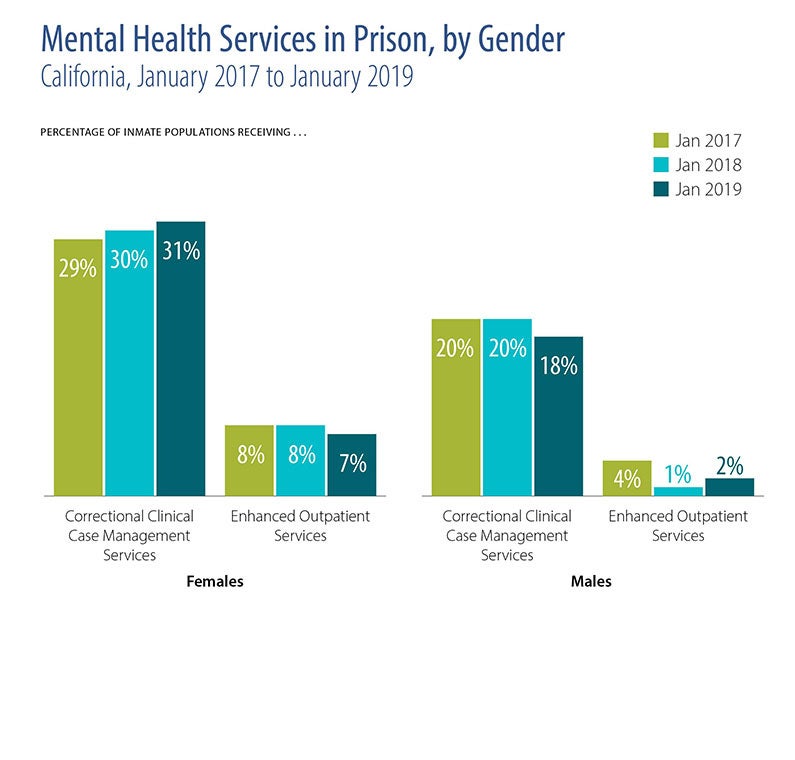
- People incarcerated in California’s jails and prisons have high rates of mental illness. In 2019, 30% of female prison inmates and 20% of the male prison population received mental health treatment while incarcerated.
The full report, a quick reference guide, and all the charts found in the report are available for download below. In addition, serious mental illness prevalence by county files are available for download as a data file.
The full report, charts, and data file are available for download below. These materials are part of CHCF’s California Health Care Almanac, an online clearinghouse for key data and analyses describing the state’s health care landscape. To see past editions of this almanac, contact us.