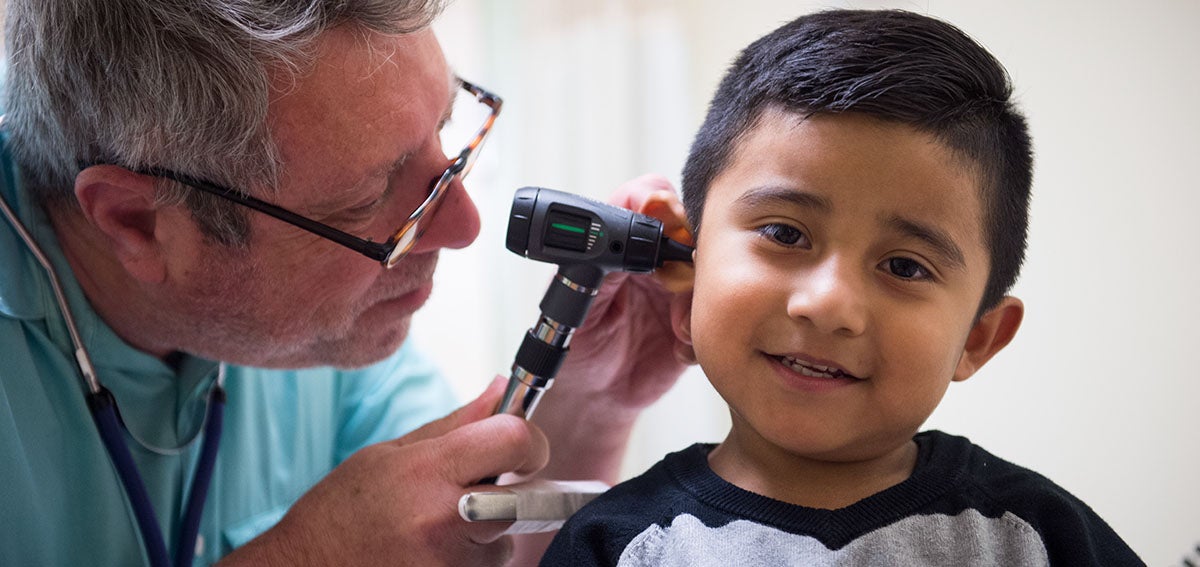
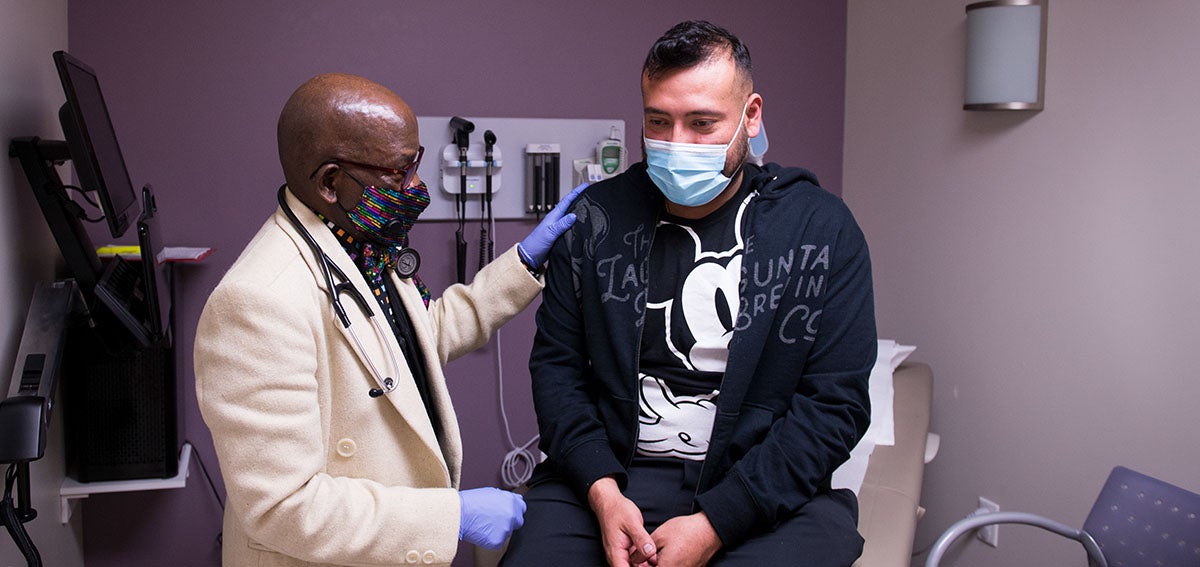
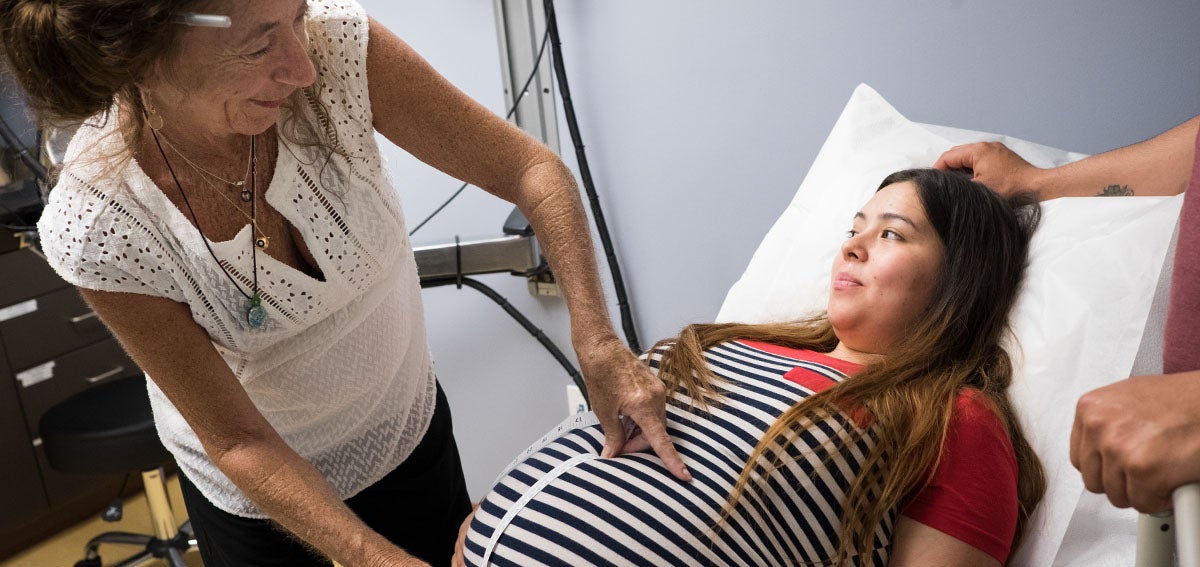
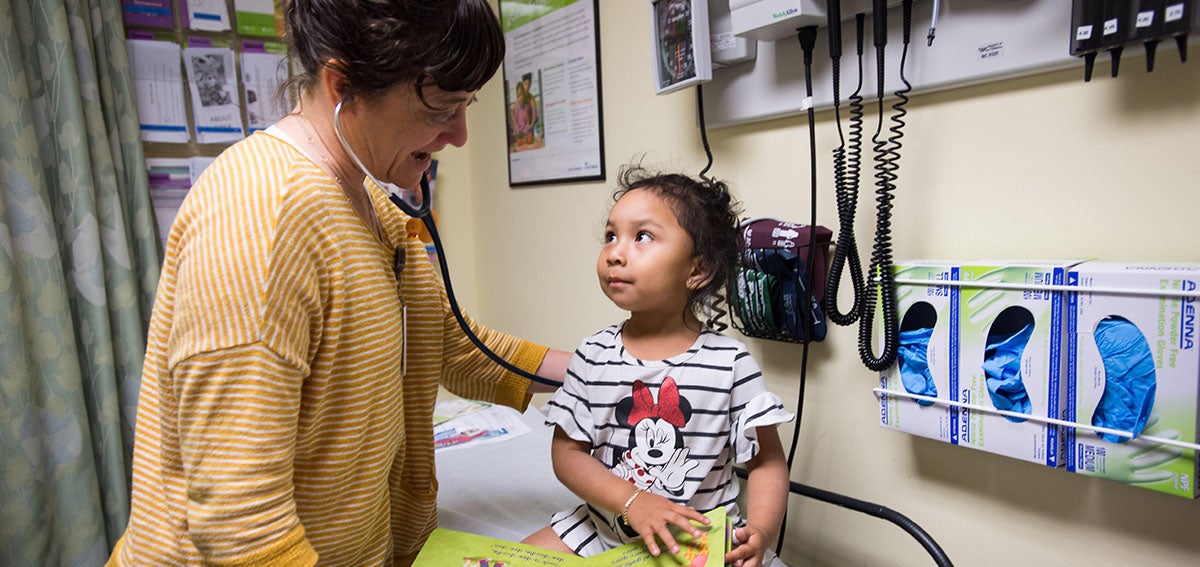
The opioid epidemic has focused national attention on the ravages of addiction. But another group of people has also been harmed by opioid overprescribing: patients with chronic pain who have become dependent on opioids.
While prescribers now face pressure to choose alternatives, many clinicians practicing in safety-net settings find their hands tied. Opioid medications may cause harm, but other choices are limited. County health systems often find their patients don’t have access to alternative and complementary therapies.
Supporting Patients with Chronic Pain
In an effort to address this gap, Los Angeles County trained health care providers to conduct brief interventions to support patients with chronic pain in making lifestyle changes. Clinical psychologist Dr. Joan Broderick with the Center for Social and Economic Research at the University of Southern California taught a curriculum known as Pain Coping Skills Training (PCST). This training is a set of evidence-based strategies and skills that health care providers can use to teach their patients to reduce the pain, fatigue, and emotional stress that accompany a chronic pain condition.
Providers trained in PCST learn to teach patients how the mind and body are linked, and how the mind can be used to quiet the pain response. While most patients experience their pain condition as entirely uncontrollable, learning about what some call the “mind-body connection” reduces patients’ sense of helplessness. They also begin to learn how to observe factors that increase or decrease their pain. In PCST, providers learn motivational interviewing, brief action planning, somatic relaxation training, activity pacing, and coping with negative thoughts and body sensations.
PCST has been shown to be effective in a wide variety of pain conditions. When patients are taught these skills, they use less medication and their quality of life improves. CHCF supported the series of two-day workshops.
Seventy-nine Los Angeles safety-net providers took the PCST training, including physicians, physician assistants, nurses, social workers, occupational and physical therapists, psychologists, and rehab peer mentors. Follow-up surveys showed that more than 900 patients received motivational interviewing and/or brief action planning by these providers within the context of a health care visit.
Implementation challenges were mainly related to time. It is faster to write a prescription than it is to teach coping skills.
Get Support for Your Organization
Under the CHCF grant, Broderick’s team is available to collaborate with interested California health systems to provide PCST workshops throughout 2018. Potential partners may contact Broderick directly.