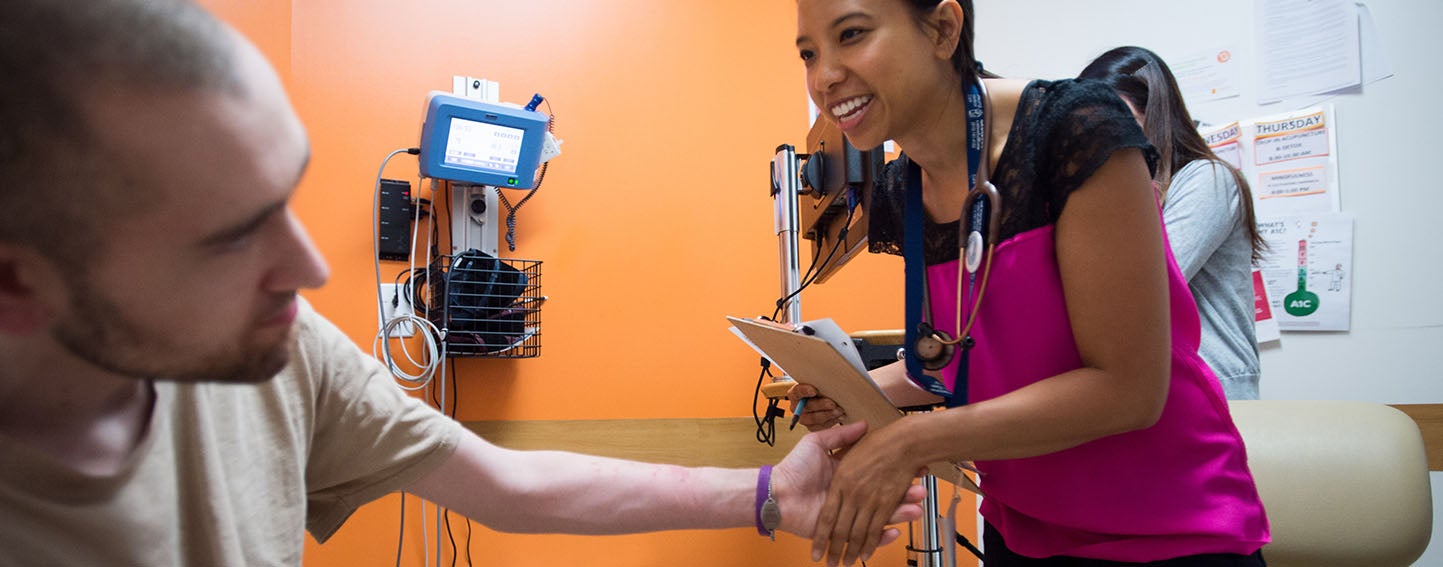
Listening to Californians with Low Incomes
Between 2019 and 2021, CHCF funded a major research project to better understand the health care experiences, needs, and values of Californians with low incomes, including understanding changes during the COVID-19 pandemic. Learn what we learned by listening to Californians with low incomes.
Over the last few months, I’ve had the privilege of listening to more than 100 Californians with low incomes talk about their experiences and aspirations in the health care system. One takeaway from those conversations rises above everything else I heard: They want to be treated as whole people, not as symptoms, visits, or poor people.
The focus groups and interviews we’ve been conducting in recent months were part of a CHCF-funded research project launched last spring to better understand the health care experiences and priorities of Californians with low incomes. (You can read this Q&A from our CHCF blog for more background on the project.) Focus groups are panels with diverse participants led by a professional moderator who facilitates conversations that provide insights into individuals’ experiences and attitudes on a given topic.
CHCF isn’t the first to explore how people experience health care in California, but there are important ways we wanted to dive deeper. Some of the existing data about care experiences and priorities are not available, not segmented by poverty level or insurance status, or are examined using only qualitative or quantitative analysis. This listening project is a powerful complement to existing research because it weaves together qualitative and quantitative work to tell a story about people’s experience of care, with a focus on those who have low incomes.
Twelve Focus Groups Around the State
In the first phase of this effort, we listened in an open-ended way to people enrolled in Medi-Cal, especially those who use California’s safety net, including community clinics and public hospitals. Medi-Cal is the backbone of the state health care system for residents with low incomes. We asked about what kind of relationship the residents have with their primary care provider, what their recent health care visits were like, and what factors determine whether the care meets their needs.
Our grantee, NORC at the University of Chicago, conducted 12 focus groups in four California counties — Alameda, Los Angeles, Shasta, and Stanislaus. They included people who identified as Black or Latino or spoke Spanish or Chinese. We also conducted nine individual interviews with people who primarily speak Vietnamese.
Even though most participants were Medi-Cal enrollees, some were uninsured, and over the course of a year many moved back and forth among Medi-Cal, employer-based coverage, and being uninsured. We recruited panelists, including some with chronic conditions, who received care in the recent past from community health centers and/or public hospitals. We tried to ensure that each group represented a mix of people who got their care from more than one provider.
Here are three of the themes that came up across the listening sessions:
“Treat Me as a Person”
In every group and interview, multiple people said that they want to be treated not as a patient but as a person. They want to feel respected and know the provider is listening. They want providers to treat them as individuals and to demonstrate compassion. People were clear about wanting not to feel judged. People with low incomes encounter stigma in so many parts of life. In health care, that stigma can be life-threatening if it discourages people from making or keeping an appointment even when care is urgently needed. It can prevent people from being honest with a provider about their needs and make it less likely they will follow through on plans to improve their health.
The people in the focus groups told us they seek respect from everyone in the facility, not only their primary care provider. Five years ago, a person’s main health care interactions would have been limited to the physician or nurse practitioner. Today, team-based care is becoming the norm, and people spend more time with nurses, social workers, medical assistants, front desk staff, and other health care workers. It turns out that such interpersonal contacts, in addition to those with the primary care provider, also matter and contribute to a person’s entire health care experience.
“Treat All of Me”
Focus group participants expressed frustration with the system being driven by volume rather than quality. Many people told stories about not being able to address more than one health issue in a single visit. Having to schedule multiple appointments on different days was a particular source of significant dissatisfaction. Several participants told us their providers felt rushed and told their patients they could spend only 10 minutes in a visit because of how they were reimbursed. But it’s also worth noting that people also said they loved it when they could see the doctor or nurse practitioner and go to the lab or pharmacy at one facility in a single visit.
For people with low incomes, having to make multiple visits is not merely an inconvenience, it’s a hardship. Most don’t have jobs with paid sick time. Many don’t have access to child care. In many cases, a trip to the doctor requires that they ride multiple buses. For people in rural areas, it means driving long distances. Each of these extra burdens takes dollars from limited paychecks and adds stress, neither of which enhances a person’s health.
“Don’t Just Give Me a Pill”
People consistently said they want their provider to focus more on preventing illness and helping them stay well. Most focus group members said the system is incentivized to concentrate on symptoms instead of root problems. People said their providers offered prescriptions as a shortcut instead of offering more meaningful care. Meanwhile, the management of multiple prescriptions with different refill timelines, different contraindications, and varying cost considerations added more layers of complexity to patients’ lives.
What we’ve been hearing has everything to do with how the health care system is designed. People see a system that they believe prioritizes volume over value, and human social interaction with providers matters far more to patients than system incentives allow.
Much work lies ahead in this fascinating project, but the listening so far has underscored the importance of having a safety-net system — built on a foundation of care, compassion, and respect — that allows and encourages providers to focus on the whole person.
Authors & Contributors


Jessica Brandi Lifland
Jessica Brandi Lifland is a freelance photographer, instructor of journalism at City College of San Francisco, and mother. Her work with publications and nonprofits such as Operation Smile, Tostan, and the California Health Care Foundation has taken her all over the world, including West Africa, the Middle East, Kosovo, Burma, Haiti, and South America.
For two decades she has been photographing the National Cowboy Poetry Gathering and has been working on a long-term project documenting the lives of the cowboy poets of the American West in affiliation with the Western Folklife Center. She plans to make her project into a book.





