Editor’s Note: This is part of a series of articles on “The Big Shortage” in California’s health care workforce. Watch The CHCF Blog for more discussions of how the workforce is changing in response to care innovations and demographic trends.
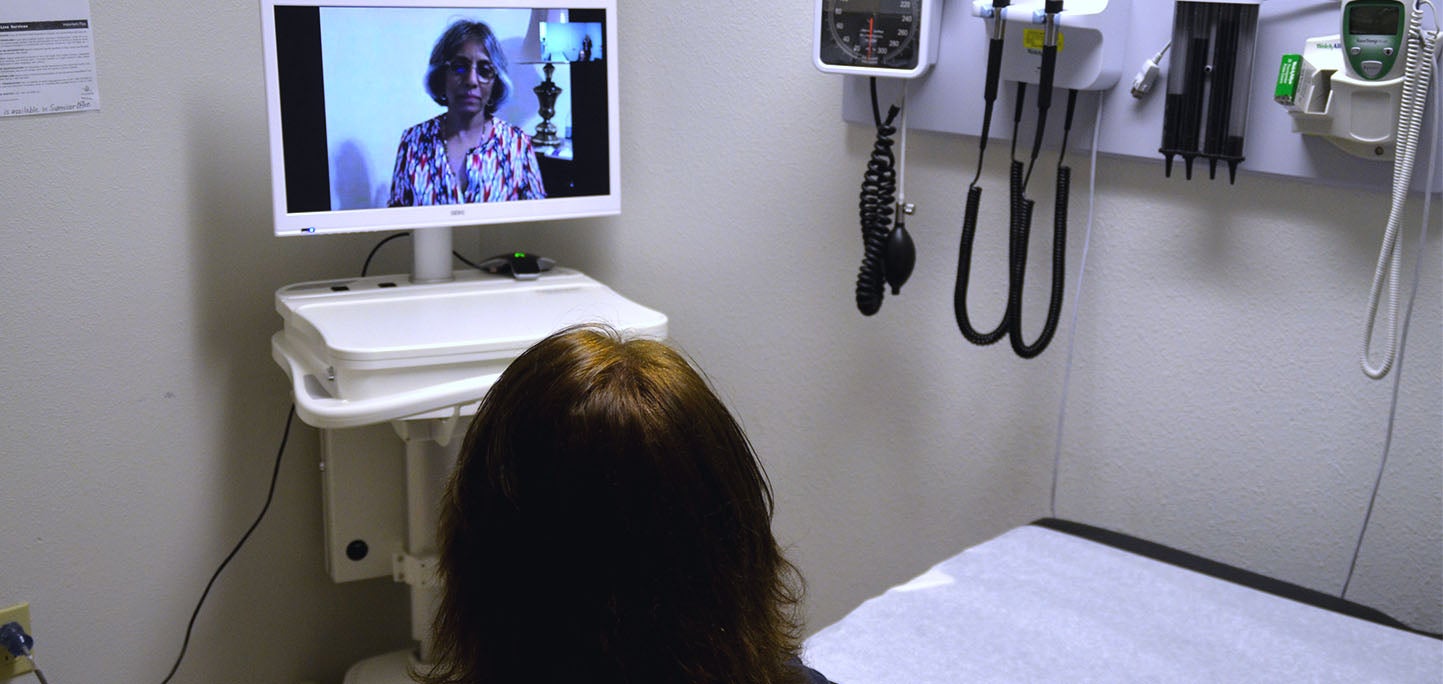
When Sally Rogers walked into the examination room at Ampla Health’s Lindhurst Clinic in tiny Linda, California, recently, psychiatrist Jothika Manepalli, MD, was waiting for her — on a wall-mounted TV monitor in the corner.
Rogers, 52, has been through a lot in the last several years. Her daughter was killed in a 2013 car crash caused by a drunk driver, and three years later her longtime partner died of a heart condition. The grief never seems to end, she said, and it’s why she suffers from insomnia and panic attacks that once led to her being hospitalized. (We changed her name to protect her privacy.)
Last year, Rogers’ primary care physician at the clinic urged her to start seeing a therapist and to work with a psychiatrist, who could prescribe medication and monitor her condition and medical needs. “He told me it would be someone on a TV, and I didn’t like the idea at first,” Rogers said. “It seemed weird.”

Rogers’ video session with Dr. Manepalli was one of a growing number of medical visits conducted through technology called telehealth (also known as telemedicine) that enables doctors and other care providers to treat people who live in places where medical specialists are in short supply. According to the American Telemedicine Association, about 1.25 million patients were treated remotely using this technology in 2016.
“In the past, patients traveled to the doctor,” said Peter Yellowlees, MD, a professor of psychiatry at the University of California, Davis. “Now the doctor can travel to the patient, virtually.”
Using telemedicine to ease the shortage of health care professionals is not just a matter of employing the right technology. It also requires changing the way health care is organized, and bringing on new categories of health care workers who can help a revamped system work more effectively.
Yellowlees helped design a pioneering telehealth program at UC Davis and in 2011 cofounded HealthLinkNow, a virtual group practice that enables psychiatrists and therapists to connect with and treat patients by video.
A Psychiatric Services Desert
Rogers, who works as a cashier, is a third-generation resident of rural Yuba County, which lies some 130 miles northeast of San Francisco. She has friends and knows lots of her neighbors, but there are no local psychiatrists she can turn to for help. Ampla Health, for example, has no onsite psychiatrist. And according to the local medical society, the entire county has no psychiatrists, and nearby Yuba City (which, confusingly, is in Sutter County) has only five. Yolo County, a suburban area west of Sacramento, has been trying to recruit a psychiatrist to its health department for four years and still can’t find one despite four salary increases, said Karen Larsen, the county’s health director.
“The shortage of psychiatrists is an escalating crisis,” said the physician search firm Merritt Hawkins in a 2017 report. The National Council of Behavioral Health also found that 77% of US counties report a severe shortage of psychiatrists. The problem isn’t strictly rural. Many low-income, inner-city communities also lack enough psychiatrists to meet their needs.
That shortfall is likely to worsen, Yellowlees said. Today, 45% of California’s psychiatrists are over 60 years old, according to a recent report from the Healthforce Center at the University of California, San Francisco. Many of these doctors will be retiring in the near future, Yellowlees said. By 2028, the Healthforce Center projects, California will have 41% fewer psychiatrists and 11% fewer therapists, social workers, and counselors than is required to meet its needs.
Geographic Factors Worsen the Shortage
Another problem is the mismatch between where most doctors are located and where they’re needed. The biggest demand for psychiatrists is in primary care clinics, hospital emergency departments, and correctional facilities, where enormous numbers of inmates struggle with mental health. While jails and prisons often are located in remote rural communities, most psychiatrists are in urban and suburban areas, and they tend to work in academic medical centers or large health systems (like Kaiser or Sutter Health).
Ampla Health, a CHCF grantee, has embraced telemedicine in a big way, said Cindy Snelgrove, MSN, MBA, its director of clinical services. Today, some 600 patients a month are seen by specialists via videoconferencing in the nonprofit’s 13 rural California health clinics. Five hundred of these visits are with psychiatrists provided by Iris Telehealth, an Austin, Texas–based telepsychiatry firm; rheumatology and endocrinology appointments are the next most common, Snelgrove said.
Ampla Health has started a program to scan the retinas of diabetic patients and then forward the images to an ophthalmology clinic at the University of California, Berkeley, where they are checked for signs of diabetic retinopathy, a complication of diabetes that can cause blindness. Primary care doctors at Ampla Health clinics also consult with numerous other specialists, sending charts and images electronically to get treatment recommendations.
Technology to Extend Expertise to Where It’s Needed
By the end of March, Ampla Health’s Yuba City pediatric clinic plans to start a dental program to address the growing number of kids who can’t obtain regular dental care. Children coming to see the pediatrician can be seen by a registered dental assistant who will do basic cleaning and take pictures. The images will be forwarded to dentists elsewhere who will suggest needed follow-up.
All of this has necessitated that Ampla hire a telemedicine adviser and two assistant coordinators, Snelgrove said. “We started growing so much, we had to hire,” she said. “We could see more patients via telemedicine, but we’re maxed out right now.”
Telemedicine enables community clinics that need a specialist for just 8 or 15 hours a week to get them virtually, said Javeed Siddiqui, MD, MPH, an infectious disease specialist and cofounder of Telemed2U, a privately held firm based in Roseville, California, that provides medical specialists by video. “We’re able to meet that economic reality,” Siddiqui said. “Our specialists work in five or six places. We string all those together and they’re working from their own office, not driving all over the place.”
While telemedicine can take different forms, at its simplest level it can enable a patient and doctor to see each other, talk, and ask questions — all that’s needed for most psychiatry appointments. For more complex visits, high-quality cameras and devices linked to the computer allow a remote physician in, say, Davis, to listen to the heart and lungs of a patient in Eureka, or to peer into their ears or throat. Providing these services also requires new kinds of workers who can set up video calls and coordinate the flow of information between patients, primary care doctors, and specialists.
“We are seeing a growing role for telehealth coordinators,” said Eric Brown, MBA, president of the California Telehealth Network, a nonprofit group supported by the Federal Communications Commission and private foundations (including CHCF) that promotes access to health care through telehealth and related technologies. These coordinators — Yellowlees calls them “virtual care navigators” — are nurses or mid-level medical assistants who schedule patient visits, gather records, set up equipment, and follow up with patients between visits.
Titles Are Less Important Than Responsibilities
Whatever they’re called, their numbers are growing, and they perform a vital role, said Siddiqui. He recalled the case of one California clinic that declined a telehealth coordinator’s request for a pay raise. She left and was replaced by another person who didn’t have the passion or skills for the work. The clinic quickly went from seeing 40 patients a month via telehealth to 10. “It proved to the clinic administrator how important the role of telehealth coordinator is,” Siddiqui said. The coordinator was rehired and given the raise she asked for.
Yellowlees argues that telehealth and related technologies can be key to expanding care to underserved communities and to improving the quality of care. “With appropriate incentives and technology support, you can take the present number of psychiatrists and redeploy them to care for a more needy population,” such as residents of underserved, low-income communities, both rural and urban, he said. “You can also increase their effectiveness by organizing care more along a planned, population health–based model.”
In this model, he said, psychiatrists work as part of a team of doctors, nurses, social workers, and others in the primary care setting. The psychiatrists act more like consultants, reviewing cases and advising but not seeing each patient.
“The traditional role of psychiatrists is to see each patient many times and follow up with them,” Yellowlees said. “That means they don’t provide care to many people because they do everything themselves. If you work with a team, you can supervise care for many more patients, rather than directly provide all the care yourself.” He believes psychiatrists “could easily see twice as many patients as they do now” by working as part of a team.
Sally Rogers said she’s gotten used to seeing Dr. Manepalli by video and that it no longer feels so strange. She’s still in a lot of distress, she said, but is sleeping a little bit better. The hardest part, she said, was during the three months she had to wait to get her first appointment with the doctor.
“During those three months, I felt like I was going crazy,” she said. “I was totally ready to give up. Now, I’m not ready to give up. I’m trying to push on.”
Authors & Contributors

Rob Waters
Rob Waters is an award-winning health and science writer whose articles have appeared in BusinessWeek, Mother Jones, Stat, San Francisco magazine, the San Francisco Chronicle Sunday magazine, the Los Angeles Times, and many other publications. He is the founding editor of MindSite, a digital publication covering mental health news scheduled to launch in fall 2021.



