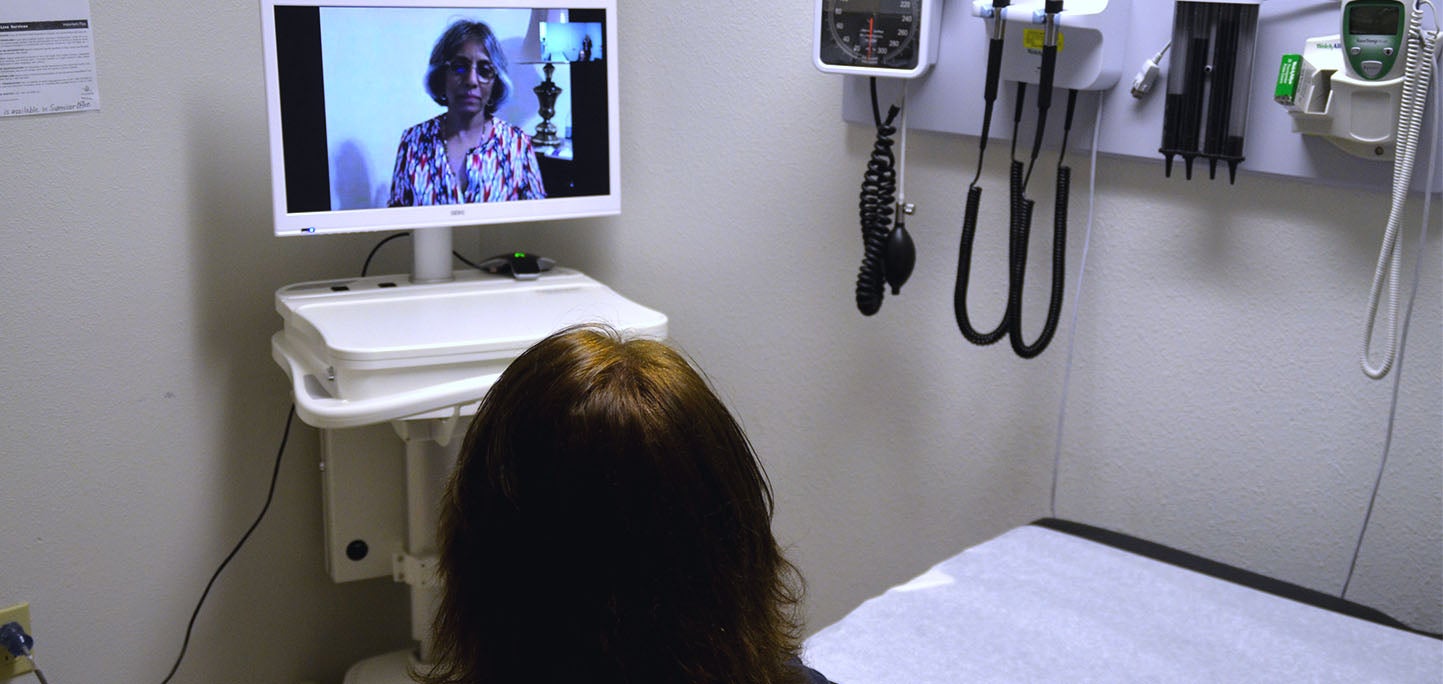
In the last week, news organizations have been sharing the story of a woman who learned about her grandfather’s bleak prospects for survival from a doctor on a video screen that was wheeled into his hospital room. As her story demonstrates, video visits — sometimes referred to as telehealth — are not always equal substitutes for in-person, human-to-human connection.
The coverage prompted me to reflect on the role of technology in these situations and how we can go about striking the right balance. It also left me with more questions about what actually occurred, including:
- What conversations had providers had with this patient and his family in the preceding weeks and months, including during his several recent hospitalizations?
- What was communicated about the patient’s prognosis, and what was heard by the patient and family?
- Would that video visit have gone differently if the provider on the screen was someone the patient and family already knew and trusted?
- Were alternatives to the video visit available, such as waiting a few hours for an in-person discussion with a provider skilled in difficult conversations? Or would missing out on a frank conversation about prognosis have led to the patient being offered additional treatments, with more burden than benefit, or being transferred to the intensive care unit as his symptoms worsened?
The Backstory Matters
The context of what came before the video visit in the story matters — regular conversations about how a disease is likely to progress and about what’s most important to the patient can help them and their family prepare for what’s coming.
What caught my attention in this patient’s story was the all-too-common cycle of repeat hospitalizations in the last few weeks of his life and the apparent missed opportunity for better, earlier communication about his prognosis. Given his declining health, a conversation about hospice would have been appropriate well before this video visit, and it may have occurred — we don’t know.
By contrast, the news coverage has focused on the role that the mode of communication — the video visit — played in this family’s care. Video visits between health care providers and patients, which are becoming more common in the US, can provide greater access to behavioral health and other specialists and can be used to let people visit the doctor from the comfort of home. These technology-enabled visits can be critically important to people in rural communities who live great distances from the nearest provider.
Today, increasing numbers of organizations provide video visits to people with serious illness, helping them address pain and symptoms while managing the emotional stress of their illness. Sometimes providers alternate video and in-person visits; or depending on the geographic distance between patient and provider, video calls might be how they usually meet.
Anecdotally, clinicians I know who provide serious illness care via video say these visits are well-received — patients are grateful not to have to travel for care. Providers feel they get a more personal glimpse of their patient’s lives by seeing them in their home environment. The initial awkwardness of talking via screen seems to dissipate quickly.
The Role of Technology
Even for people who are quite ill, video visits can work well and include family members at a second distant location. In such instances, technology solves a problem.
But technology isn’t always the complete answer. Video interaction has the potential to make care more patient-centered or more impersonal depending on how it is used.
What happens before, during, and after a video meeting determines whether the technology is an acceptable and effective vehicle for a particular conversation. It may seem perfectly appropriate in some circumstances for family members to communicate by video with a provider they haven’t seen before. At other times, it may feel impersonal and unacceptable.
It is up to the health care community, with input from patients and families themselves, to identify and understand the difference.
Authors & Contributors




