When I joined the California Health Care Foundation a year ago, the organization had a 20-year track record of making health care work better for all Californians. In large part, my job was to help colleagues figure out how to maximize CHCF’s impact, given the rapidly changing world around us. Armed with flip charts, sticky notes, and a fantastically talented team, I spent much of the last year working with our board and staff to ask the hard questions about our priorities, align us around our goals, and refine our strategy to deepen our impact.
In her annual President’s Message earlier this month, CHCF president and CEO Sandra Hernández did a great job of articulating where we ended up: “Too many Californians with low incomes are held back or suffer because it is too hard to get the care they need. . . . The foundation’s top priority should be to address that problem.” Now my job is to help CHCF make good on that promise. It is critical to our success that our partners and other stakeholders understand what our strategic priorities mean in practice.
CHCF’s new priorities represent a sharpening of focus rather than a material pivot from the work we have been doing over the past few years. The first thing our partners may notice is that many things remain the same, including our mission, our focus on driving change in the health care delivery system, and our multifaceted approach to reaching our goals, including grants, policy, communications, and program-related investments. Our partners may notice that our frame is shifting; we will have a more intentional and dedicated focus on making the health care system work better for Californians with low incomes. We will support this focus with clearer criteria for entering new bodies of work and better articulated strategies for accomplishing our goals (including what we are trying to achieve over what time period, how we believe we can help drive change, and how we will know when we are successful).
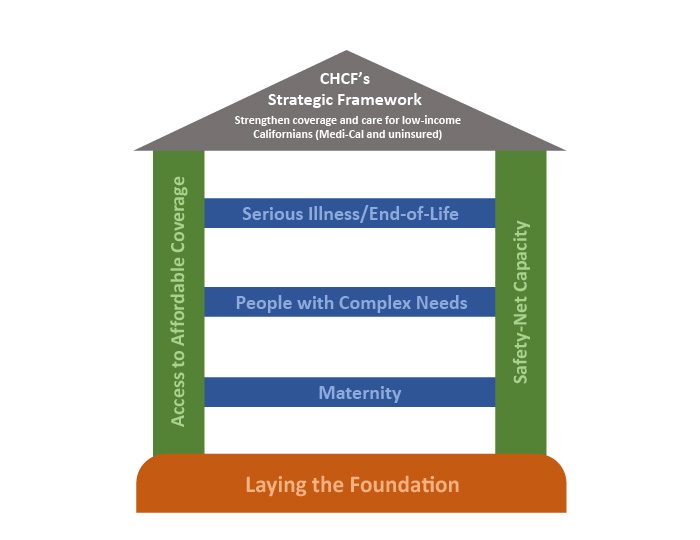
You can find more about our new strategy and about our criteria on our Learning & Impact page. In the coming weeks, we will elaborate on each of our focus areas in a series of articles on The CHCF Blog. In the meantime, here’s an overview of how we will target our grantmaking in the next few years.
Improving Access to Coverage and Care
We believe that all Californians should have health coverage and that the state policies and programs should ensure that Californians with low incomes are able to get the care they need, when and where they need it, and at a price they can afford. That means finding solutions that get California to universal coverage. It also means strengthening the Medi-Cal program, which is indispensable to California and offers us one of the best opportunities for improving the well-being of seniors with low incomes, persons with disabilities, children, and adults.
Through our efforts to improve access to coverage and care, we aim to transform the health care safety net so it can provide timely, high-quality care that meets patients’ needs. We will focus especially on helping community health centers and public hospitals manage population health (including the adoption of value-based payment systems), modernizing the health care workforce (including our support for the California Future Health Workforce Commission), and expanding the use of telehealth, the use of telecommunications tools and infrastructure to connect patients with providers and improve access to care.
Promoting High-Value Care
We believe that health care systems must deliver high-value care to Californians with low incomes. In reviewing our high-value care portfolio, we started with data: What are the biggest cost drivers in Medi-Cal? Where are the inequities? Where can CHCF and our partners make a difference? We chose to focus on areas that are either high volume in the safety net (like maternity care) or where patients face disproportionately poor outcomes despite receiving high-cost services.
A centerpiece of our strategy is improving care for people with complex needs. People with mental illness or substance use disorder die at a much younger age than their peers and are disproportionately represented in the 5% of people in Medi-Cal who account for 50% of Medi-Cal spending. Medi-Cal and safety-net providers aim to improve these grim statistics with care that addresses physical, behavioral, and social needs. CHCF is working with partners to support better data exchange and measurement, as well as policies and new payment models supporting care integration.
Given that half of all babies born in California start their lives with a Medi-Cal card, maternity care will continue to be an important focal point. We celebrate the successes of our partners in driving down cesarean-section rates (the statewide average for low-risk, first-pregnancy c-section rates has dropped from 26.5% to 25.1% since 2015 — the first downward trend in 20 years). Next we will turn our attention to perinatal depression and anxiety, which disproportionately affect mothers with low incomes and their families. And we are exploring how to address the significant disparities in outcomes for African American mothers.
Finally, we will keep building on our deep experience in care for people with serious illness and those approaching the end of life. We will focus on ensuring that Californians with low incomes have access to comprehensive palliative care, including in rural and safety-net settings, and that their treatment preferences are routinely elicited, documented, and honored.
Laying a Foundation for Change
At CHCF, we often describe California’s health care landscape as an ecosystem. Just as any system in nature can only thrive if it is in balance, our health care system can only advance if it has some fundamentals in place. We have chosen to invest in four areas that help prime California for future progress.
- We provide timely market analysis and insight to ensure that health care leaders have the best available data to support informed decisionmaking.
- We support high-quality health care journalism so issues that matter to Californians are responsibly covered and openly discussed.
- We provide educational programs and collaboration networks that help clinical leaders and other partners develop the vision, capabilities, and networks to spread good ideas across the health care system.
- We bridge the innovation gap so safety-net players and entrepreneurs can better work together to improve delivery.
Our planning exercises left us with one other big takeaway: Strategy is never done. Our external environment is always changing. While some of those changes open exciting new possibilities, others create big new barriers. We must stay nimble and ready for both. And this constant change brought home to us the need to be continually listening to our partners and to Californians with low incomes to ensure that our work responds to the communities we serve.
Even with all the constant uncertainty, California has the opportunity and responsibility to improve health care for those who need it most. My CHCF colleagues and I are excited to work with our partners to turn vision and strategy into real, meaningful change.
Authors & Contributors




