
During the COVID-19 pandemic, the American public developed a deeper appreciation for behavioral health care, the umbrella term for mental health and substance use treatment. While demand for it is soaring, the US health care system is still falling far short. Despite significant spending, people with behavioral health conditions still suffer greatly. They experience more illness, poorer health outcomes, and a shorter life expectancy than the general population — often from preventable physical health conditions. State and federal governments are providing additional funds to improve behavioral health care, but measuring the quality and coordination of these services, which is needed to improve both access to care and outcomes, has always been an obstacle.
You can learn more about the Behavioral Health Quality Framework by viewing a replay of NCQA’s October 8, 2021, webinar, A National Conversation on a Behavioral Health Quality Framework for Joint Systems Accountability That Improves Care.
Health systems will be able to deliver whole-person care that addresses the full spectrum of a person’s health care needs only if the quality of behavioral health care is raised. The fragmented and inequitable state of behavioral health care calls for a quality measurement framework that can be used to guide and hold all types of health care organizations jointly accountable for improving outcomes for people with behavioral health needs. To guide development of this framework, CHCF commissioned the National Committee for Quality Assurance (NCQA) to evaluate the current behavioral health quality measurement landscape and to share insights about the needs and challenges facing behavioral health care organizations across the health care system.
Our study team reviewed 39 active federal programs, which collectively use more than 1,400 quality measures and metrics. Only 35 unique standardized behavioral health quality measures were identified across all federal programs, and of those, 16 were used in only one program. The broad array of behavioral health quality measures used in federal programs mostly focus on processes related to narrowly specified conditions or treatments (e.g., depression screening) and leverage administrative claims data. In contrast, outcome measures that would allow programs to measure whether patients were achieving treatment goals were extremely underrepresented.
Existing Reporting Measures Are Insufficient
Our team spoke to stakeholders from various levels of the behavioral health care delivery system within five state Medicaid agencies, including California. These stakeholders reported that existing quality reporting efforts were both burdensome and insufficient for driving improvements in care. A large number of misaligned measures cover subsets of the overall population and lack standardized outcomes. As a result, stakeholders report that it is challenging to articulate the overall quality of care for patients or to make valid comparisons across different programs or systems.
In Behavioral Health Quality Framework: A Roadmap for Using Measurement to Promote Joint Accountability and Whole-Person Care, we propose a blueprint for improving behavioral health quality and promoting joint accountability across all entities serving people with behavioral health needs.
In this framework, each level of the delivery system — state and federal governments at the top, managed care organizations (MCOs) in the middle, and providers and facilities at the base — uses only the performance measures and metrics most relevant to its role in the delivery system. This approach reduces the redundancy and overall number of quality measures used within a system and ensures that quality measures at each level of the system drive meaningful improvements in care.
For example, if a state sets a goal of reducing opioid-related deaths, it would use a bundle of quality measures and metrics that might include concepts such as maintenance of a prescription drug monitoring program (structural measure), follow-up after emergency department visit for opioid overdose (process measure), and opioid-related mortality (outcome measure).
The state would be explicit about this goal in contracts with MCOs and in the state measure bundle being used to track its success. In turn, MCOs would be responsible for using their own unique but coordinated bundle of measures. Those MCO measure concepts might include behavioral health network adequacy (structural measure), opioid use disorder treatment continuity (process measure), and repeat overdose events (outcome measure).
At the facility or provider level, relevant quality measure concepts might include the number of providers within a practice authorized to prescribe buprenorphine (structural measure), patient access to medications for the treatment of opioid use disorder (process measure), and patient treatment dropout rates (outcome measure). The use of the term “measure concept” is intentional, as standardized measures that meet stakeholder needs may not yet be available. Stakeholders should make consensus-based decisions about where new measures may need to be positioned within the system to assess meaningful aspects of care.
To support implementation of the BH Quality Framework, the team proposes a roadmap that includes three primary components, outlined in the figure below.
Roadmap to Joint Accountability for Behavioral Health
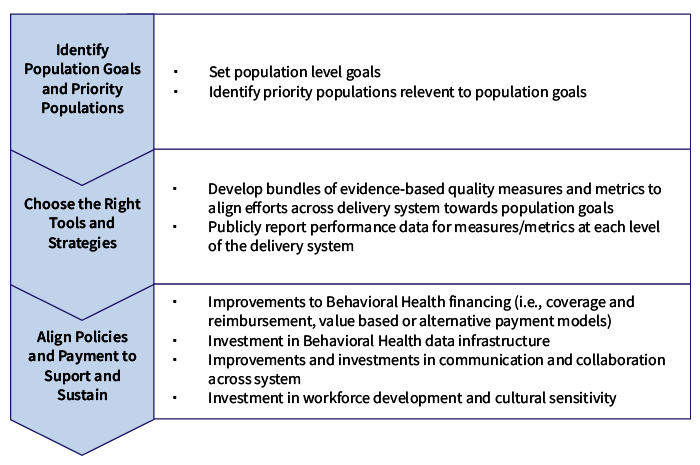
Federal and state governments have made substantial investments in behavioral health, particularly as COVID-19’s substantial impact on mental health and substance use have come into focus. To realize the value of these investments, we need to measure access, quality, and outcomes — and to have a clear approach and solid framework for doing so. The study team believes this model can simplify and streamline federal and state quality oversight requirements — and help to align and coordinate efforts to improve people’s behavioral health care. Further, the team believes this framework can promote collaboration and joint accountability for whole-person care, even among systems with differing ways of financing behavioral health.
Authors & Contributors

Serene Olin
Serene Olin, PhD, is assistant vice president of research and analysis at the National Committee for Quality Assurance. She leads and manages NCQA’s behavioral health research portfolio, which is aimed at using measurement tools to improve behavioral health care quality in delivery systems.

Lauren Niles
Lauren Niles, MPH, is a senior research associate at the National Committee for Quality Assurance. She leads and oversees NCQA’s behavioral health quality measurement HEDIS portfolio and participates in research related to behavioral health care quality and delivery.

Matt Chinworth
Matt Chinworth is an illustrator based in Tulsa, Oklahoma. His work has appeared in many major publications, including the New Yorker, The Atlantic, New York Times, Washington Post, Boston Globe, Politico, Christianity Today, Fast Company, and Harvard Business Review.





