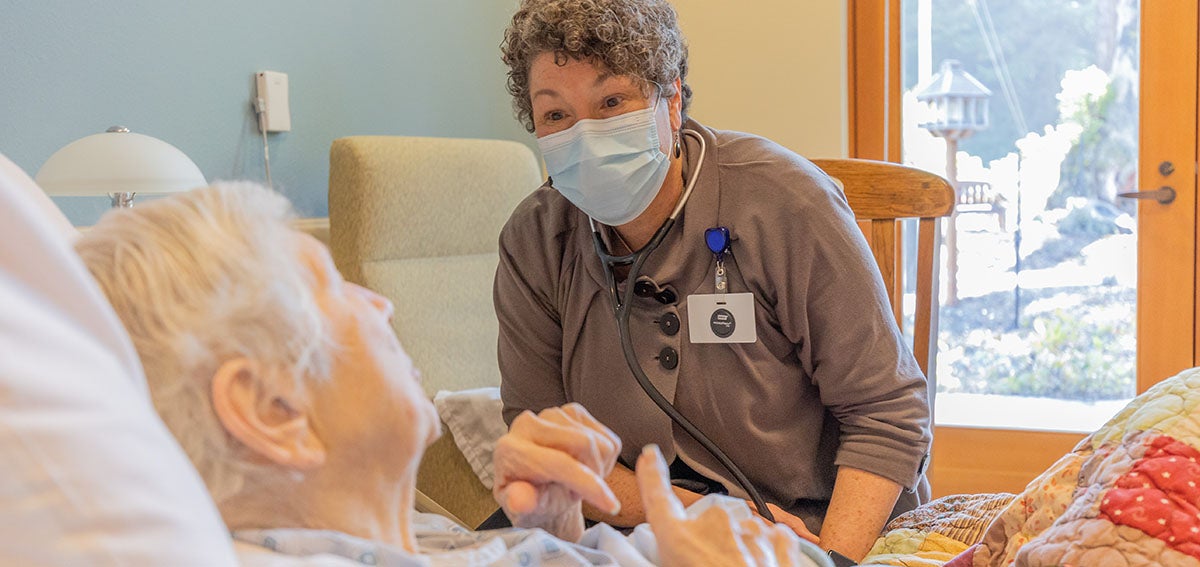
When a woman recently called the Priority Care Center clinic in Eureka, California, because she was struggling with depression and suicidal thoughts, nurse practitioner Karen Ayers knew the patient would need more than the standard 15-minute primary care slot. During an hour-long appointment, the patient, who was in her sixties, cried as she confided that she was eating fast food instead of cooking and spending days in bed. She told Ayers that she didn’t deserve to be depressed because she had food, shelter, and a loving husband.
Based on the patient’s history, Ayers suspected alcohol use was exacerbating the woman’s chronic depression, and the patient’s daughter confirmed that suspicion. Ayers, who recently completed a psychiatric and mental health nurse practitioner program, worked with the woman and the daughter to create a plan to taper the alcohol use, switch to a different antidepressant, and see one of the clinic’s wellness coaches for help in changing her daily routines. The woman soon stopped drinking alcohol and having suicidal thoughts, and now she cooks, takes regular walks, and says she feels more joyful.
In contrast to other types of providers, Ayers had the flexibility to spend more time with the patient and offer enhanced services, including home visits and lifestyle coaching, because the goal of her clinic is to provide holistic care to underserved populations. When the clinic opened its doors in 2016, it started with two registered nurses, a medical assistant, two wellness coaches, and a physician medical director. At the time, many Humboldt County residents were relieved to find a clinic that accepted new patients.
Scarce Physicians
The steep demand for primary care services in the county motivated the Priority Care Center to eventually hire three more nurse practitioners (NPs) and plan for more. But current state regulations limit one physician to supervise no more than four NPs. Doctors are growing increasingly scarce in her rural community, said Ayers, who has lived in Eureka for more than 30 years and has had training in acute care, primary care, hospice care, and palliative care nursing.
“When primary care physicians retire, there is nobody to backfill,” she said. “We have a revolving door of younger physicians who will work temporarily in underserved areas to gain loan repayment benefits, but they often leave once their obligation is met.” With the existing physician supervision requirements, the shortage of doctors directly restricts the team’s ability to hire more NPs.
In 2020, California governor Gavin Newsom and the state legislature enacted a law (AB 890) that will allow nurse practitioners to practice without physician supervision once they meet certain criteria.
Research has shown that the quality of primary care provided by NPs is similar to care delivered by physicians. Most states already allow NPs to practice independently, and access to primary care is greater in those states. California faces a projected shortfall of 4,100 primary care clinicians over the next 10 years, so more providers are needed to meet demand.
Complexities of Bringing Law to Fruition
The California Board of Registered Nursing (BRN) is determining whether established NPs will be required to take a state examination in addition to the national board examination if they seek to practice without physician supervision. The BRN also needs to define the minimum transition-to-practice period, during which an NP would develop the skills and experience needed to practice without physician supervision.
“My hope is that this rule-making process goes as smoothly as possible so that NPs can provide care to patients in underserved communities and other areas where it is difficult to recruit providers,” said Garrett Chan, PhD, NP, president and CEO of HealthImpact, an organization focused on increasing the nursing workforce.
More than 31,000 California nurse practitioners have been working with minimal supervision in clinical settings under the supervision of physicians for years, sometimes decades. These NPs fully understand the care needs and interventions required to help a patient in their health journey, and they can safely practice without physician supervision, Chan said.
California senate president pro tempore Toni Atkins (D-San Diego) has introduced SB 1375 to clarify that NPs who have been practicing for three years or more would satisfy the transition requirement. If this bill doesn’t pass, the transition-to-practice requirement will then need to be defined by BRN regulation.
Susanne Phillips, a family NP and associate dean at the University of California Irvine’s Sue & Bill Gross School of Nursing, is encouraged by recent progress toward AB 890 implementation but said she is concerned about future delays caused by protracted legislative and regulatory processes. “The primary intent of AB 890 was to increase access to care for patients, but we can’t do that until these processes are complete,” said Phillips, who has worked in leadership roles within the California Association for Nurse Practitioners and the state BRN.
Youth in Need of Services
The current restrictions on NPs are also affecting children in the Eureka area. In 2018, the Priority Care Center launched a middle school–based health center in an impoverished area where children were experiencing food scarcity and neglect. Students who sought care at the center for stomachaches or headaches would often talk to the nurse practitioner about their difficult situations at home, and she connected them with therapy and social services for support. The center became a refuge for youth, but it recently reduced services because the NP retired at the same time more NPs were needed at the Priority Care Center. The team could not hire more NPs for the school because the supervising physician already oversees the maximum four NPs under current rules.
The primary care provider shortage has taken a personal toll on Ayers. She often worked long hours after clinic closing to finish care tasks for her nearly 800 patients, and she said the stress began to affect her mental health. These challenges were a factor in her decision to pursue her interest in caring for patients in the final stages of life. In January she left the Priority Care Center to take on a new role as clinical director of palliative care services at Hospice of Humboldt. “When I worked in primary care, I had a reputation in the community for saying yes to patients who could not access care elsewhere, but it was exhausting,” said Ayers. “We desperately need to have the freedom to hire more nurse practitioners to serve this community.”
Reaching Undocumented Patients
The need for more primary care providers is acute in urban areas, too, and family nurse practitioner Cynthia Sanchez works with undocumented and uninsured patients in Los Angeles and Orange Counties, who often face significant barriers when seeking medical care.
“A lot of my patients need someone who understands their social context,” said Sanchez, a clinical assistant professor of nursing at the University of Southern California’s Dworak-Peck School of Social Work who has worked in gynecology and sexually transmitted disease (STD) clinics for county government agencies. “It does not do any good to prescribe medicine if patients do not understand why they are taking it or if they cannot afford the medication.”

She takes time to listen to patients who are struggling with fear, lack of education, and language barriers that inhibit their willingness to follow through with treatment recommendations. In Los Angeles, Sanchez saw a woman in her thirties who had been referred to surgery to remove a painful ovarian cyst, but the surgeons could not convince her to go forward with the procedure. Sanchez talked to the patient and discovered that she held deep fears of having surgery and wanted to shrink the cyst with Chinese herbal treatment. Sanchez suggested that she try the herbs for a few weeks and schedule an ultrasound to see if the treatment was working. If the cyst had grown, they could discuss the possibility of surgery.
“I took the time to listen to her reasoning and develop a plan she could accept,” said Sanchez. The ultrasound revealed that the cyst had grown, and Sanchez referred the patient back to the surgeon for the procedure.
Sanchez also has opportunities to reduce the stigma of STDs. When a middle-aged man with HIV came to the clinic, he shared with Sanchez that he was afraid of infecting his partner even though the antiviral medication had reduced his viral load to undetectable levels. He had been avoiding physical intimacy with his partner for years and felt dirty and ashamed. She explained that if tests could not detect the virus that his partner was not at risk. Sanchez connected him with a support group to help with the psychological aspects of living with HIV. A few months later he thanked Sanchez because his mood and partner relationship had improved significantly.
For Sanchez, helping patients to better understand their medical conditions and find the help they need to thrive are the reasons she became a nurse practitioner. She knows NPs are more likely than physicians to take new Medi-Cal and uninsured patients.
“I see many patients who thought there was no way to get the treatment they needed,” she said. “It is very rewarding to help them, and they are often surprised to find an advocate who is willing to listen and come up with a plan that they can follow.”
Authors & Contributors

Heather Stringer
Heather Stringer is a freelance health and science journalist based in San Jose. She studied civil engineering at Stanford University and started her journalism career at a daily newspaper in Fremont. Heather began covering health care as a staff writer and editor at a nursing magazine and launched her freelancing career in 2003. Her work has been published in Scientific American, Monitor on Psychology, Cure, Proto, and Nurse.com.

Shaun Walker
Shaun Walker is a former staff photojournalist and later also photo editor at the Times-Standard in Eureka, where he worked for nearly 25 years. He has done freelance work for the New York Times, Los Angeles Times, San Francisco Chronicle, and other major publications, as well as for local organizations. He also does wedding, nature, and portrait photography. He loves to travel the world, hike, and do whitewater and sea kayaking.

Harrison Hill
Harrison Hill is a documentary photographer and filmmaker based in Los Angeles, California. His work focuses on social justice issues centered around communities of color in the US.





