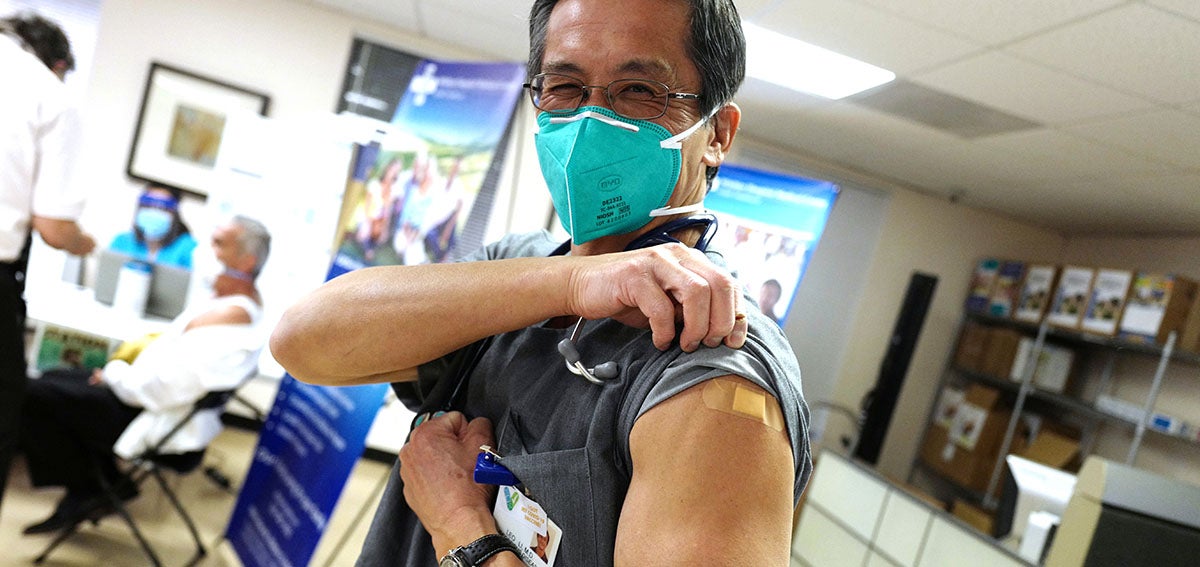
On December 14 — only 279 days after the World Health Organization declared the coronavirus outbreak a pandemic — intensive care unit nurse Helen Cordova became the first Californian to get the COVID-19 vaccine.

“I’m feeling great,” Cordova said in a video after receiving the shot from her employer, Kaiser Permanente Los Angeles Medical Center. “I’m excited. I’m hopeful. And I really encourage everyone to consider receiving the vaccine so we can start putting an end to this pandemic.”
The moment represented the culmination of nine months of work at breakneck speed to research, test, and produce a COVID-19 vaccine. The previous fastest time to develop a vaccine was just shy of five years, an achievement led by American microbiologist Maurice Hilleman, PhD, in pursuit of a mumps vaccine.
The Pfizer/BioNTech vaccine is being administered across the country, and the Food and Drug Administration granted emergency use authorization for a COVID-19 vaccine made by Moderna on December 18. More vaccines are on the way — the New York Times coronavirus vaccine tracker lists 18 vaccines in the final stages of testing.
“When all is said and done, making the vaccine might turn out to have been the easy part,” wrote the New York Times editorial board. Next, vaccine makers must ramp up production and work with transportation companies and state governments to distribute them quickly and equitably. The federal, state, and local governments must collaborate with community leaders to maximize uptake. And throughout the vaccine rollout period, public health officials must motivate Americans to continue (or begin) adhering to public health measures like mask wearing.
Challenges to Production and Transportation
Logistical challenges abound when it comes to manufacturing and distributing COVID-19 vaccines. Before the pandemic, the global production of vaccines was 3 to 5 billion doses a year, excluding the seasonal flu vaccine, Sarah Gonzalez and Alexi Horowitz-Ghazi reported on the Planet Money podcast. Effectively inoculating the world’s population against the coronavirus will require about 6 billion COVID-19 vaccine doses. Because some vaccines, including Pfizer’s, require two doses, the need could increase to 12 billion doses — nearly triple the current capacity.
After production, some vaccines must be kept extremely cold. The Pfizer vaccine requires storage at minus 94 degrees Fahrenheit, which means vaccine administration sites will need ultra-low-temperature freezers, and transportation companies will need a lot of dry ice.
Supply chain shortages are an issue when it comes to the tiny glass vials and syringes needed to store and administer vaccines. Borosilicate glass vials help protect the vaccine from contamination and high temperatures, Rebecca Heilweil reported in Recode. Schott, a German company that is the world’s largest producer of pharmaceutical glass, has ramped up production of borosilicate glass containers. But some of those vials are used for other important medications, including “all of the cancer drugs made worldwide,” Stefan-Marc Schmidt, vice president of marketing and sales at Schott, told Planet Money. “We have to make sure that these vials for those drugs are supplied as well.” Borosilicate glass is also used to make syringes.
Finally, to move the COVID-19 vaccine around the world, we need a lot of trucks and airplanes. There are about 2,000 cargo planes in the world, and Glyn Hughes, the head of cargo at the International Air Transport Association, told Planet Money we need four times that number of cargo planes to move all the COVID-19 vaccine vials. However, about 2,500 passenger airplanes have switched to cargo-only to assist with vaccine distribution — a silver lining of low travel demand during the pandemic.
A Plan for Equitable Distribution
Once vaccine doses reach their destinations, states must decide how to distribute them quickly and equitably. On December 14, California governor Gavin Newsom launched the “Vaccinate All 58” campaign, which prioritizes safety, transparency, and equity in the state’s plan to distribute the vaccine to all of the state’s 58 counties.
Two state task groups are working with the state to ensure equitable distribution of the vaccine. The Drafting Guidelines Workgroup is developing guidance for the prioritization and distribution of vaccines when supplies are limited, and the Community Advisory Vaccine Committee is providing feedback on planning efforts and resolving barriers to equitable vaccine implementation.
“What impresses me most about this campaign is the awareness that we must focus on communities that have sometimes been neglected, whether the reasons involve race, language, ethnicity, or something else,” said Anthony Rendon, speaker of the California State Assembly, in a press release.
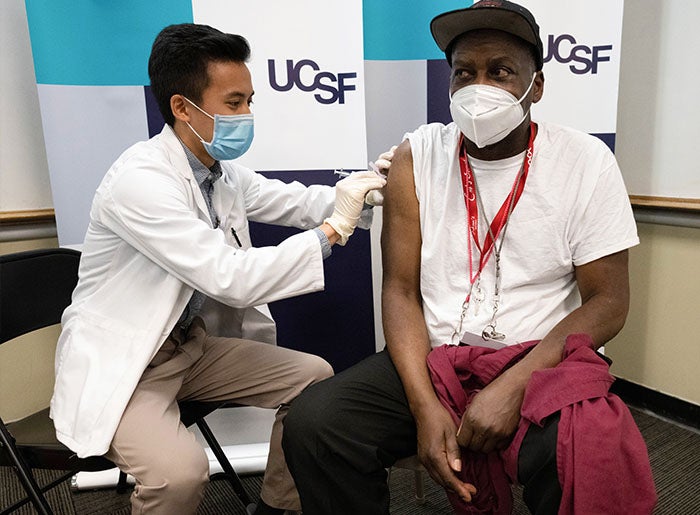
In phase 1a of the distribution plan, the California Department of Public Health recommends that health care workers and residents of long-term care settings, including skilled nursing facilities, receive the vaccine. As of December 18, California had recorded 5,852 COVID-related deaths among residents of skilled nursing facilities. This represents 26% of total deaths from COVID-19 in the state. “I don’t think there’s any question that we need to vaccinate nursing home staff and nursing home residents,” Michael Wasserman, MD, president of the California Association of Long-Term Care Medicine, told Catherine Ho and Lauren Hernández in the San Francisco Chronicle. (In July, Wasserman said COVID-19 was “the greatest threat to nursing home residents that we have seen in many years, if not ever.”)
Phase 1b is expected to prioritize essential infrastructure workers. “The frontline workers who we have asked to continue serving our economic needs — those picking the crops and working in warehouses, packing houses, transportation — have carried an unfair burden by getting the virus at higher rates because of the work they do,” Tony Iton, MD, JD, MPH, senior vice president for healthy communities at the California Endowment, wrote in CalMatters. “It is critical that they get the vaccine early to help stem the exposure rate, and out of fairness and equity.”
Public Support for Vaccination
A recent survey from KFF found 71% of Americans say they would definitely or probably get a COVID-19 vaccine — up from 63% in a September survey. The increase in vaccine acceptance occurred across racial and ethnic groups and among Democrats and Republicans (but not independents). Still, 42% of Republicans, 36% of people age 30 to 49, 35% of rural residents and Black adults, and 33% of essential workers said they would probably or definitely not get the vaccine.
“It will take effective messaging and information efforts utilizing credible messengers and digital communications techniques to reach these different groups, targeting their different worries about the vaccine,” Drew Altman, PhD, president and CEO of KFF, wrote in a column. “No one message or single messenger is likely to be effective.”
To increase public confidence in the vaccine, former presidents Barack Obama, George W. Bush, and Bill Clinton have said they will take the vaccine publicly, Heilweil reported in another Recode article. The government’s top infectious disease specialist, Anthony Fauci, MD, has also volunteered to do so on camera. Vice President Mike Pence, Second Lady Karen Pence, and US surgeon general Jerome Adams, MD, MPH, received their vaccines on television on December 18, and President-elect Joe Biden and incoming First Lady Jill Biden, EdD, will publicly receive their first doses on December 21, Alice Miranda Ollstein reported in Politico.
Community health workers and promotores (CHW/Ps) — trusted community members who serve as links to health and social services — could help alleviate fears about the vaccine, especially in Black and Latinx communities, which have been historically mistreated or excluded by the health care system. “Through good times and bad, [CHW/Ps have] earned a deep level of trust,” wrote Rishi Manchanda, MD, MPH, president and CEO of HealthBegins, and Claire Qureshi, MBA, senior director for the Community Health Acceleration Partnership, in the Hill. “That trust has been proven effective in the fight against many outbreaks and pandemic, including this one.”
Keep Wearing a Mask — with Optimism
The COVID-19 pandemic is long from over, but with the first doses of vaccines making their way around the world, there is much to be thankful for at the end of this unprecedented year. While vaccine production ramps up, it is more important than ever that people adhere to public health guidelines when interacting with others outside of their household.
The Pfizer vaccine appears to prevent symptomatic illness and severe disease, but the studies “haven’t looked at whether the vaccine prevents someone from carrying COVID-19 and spreading it to others,” said CNN medical analyst Leana Wen, MD, visiting professor of health policy and management at George Washington University School of Public Health. “We need for everyone to keep following the precautions we’ve been talking about all along. Wear a mask. Keep physical distancing. Avoid indoor gatherings. Wash your hands.”
Essential Coverage will be back in the new — and hopefully better — year.
Authors & Contributors