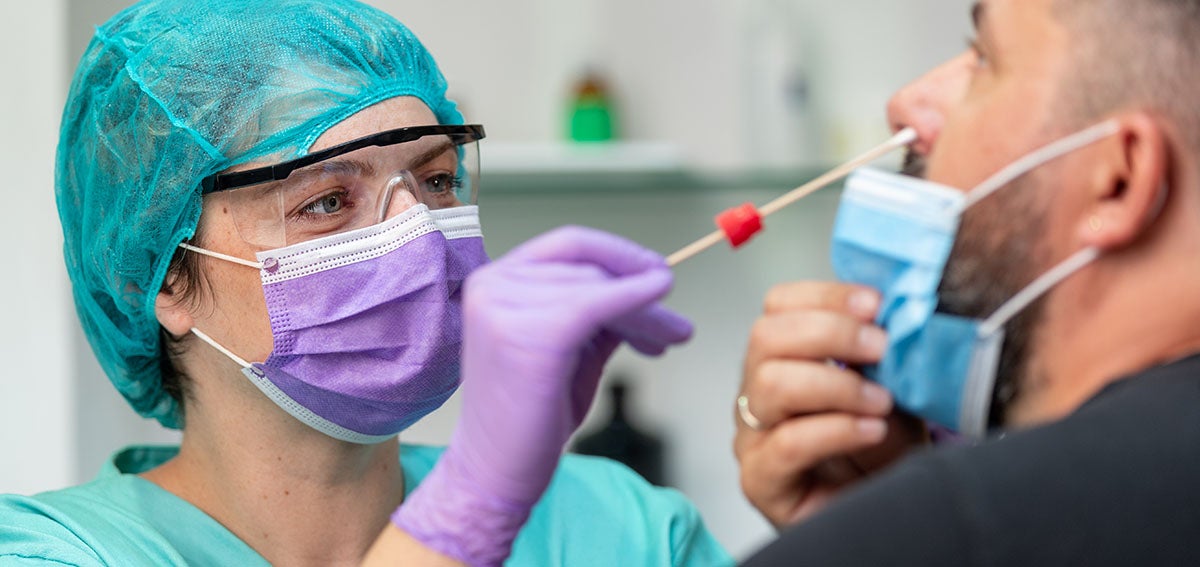

Brian Devlin wanted to be tested for COVID-19. After experiencing intermittent symptoms following his participation in a demonstration in Oakland, he wanted to take precautions before leaving his home in Richmond, California, to visit his wife in Idaho.
On July 1, he scheduled a testing appointment through the Marin County Health and Human Services Department. The first available time slot was on July 10. The test “took 10 seconds. . . . And then they assured me that I’d know [the results] in four or five days,” Devlin told ABC7.
But it took eight days for Devlin to receive a text saying his results were ready, and when he went online and typed in his last name and birth date, the system couldn’t locate the results.
Matthew Willis, MD, MPH, the Marin County public health officer (and COVID-19 survivor), told ABC7, “We have no control over that process; it has to do with private labs and their ability to obtain the reagents in order to process the samples. I agree, it’s incredibly frustrating for us as well. . . . I spent a lot of time with the other health officers discussing our mutual frustration over delays in obtaining results.”
Rapid testing is integral to the public health strategy to identify, isolate, and treat new cases of COVID-19. But from the start of the coronavirus outbreak, the US has failed to meet testing targets. In February, the US Centers for Disease Control and Prevention distributed to public health labs across the country 200 test kits — each one capable of processing up to 800 patient specimens. Health officials quickly discovered that the kits lacked critical components and delivered invalid results.
“States are duking it out for supply chains. . . . It’s the wild, wild west.”
—Blair Holladay, CEO, American Society for Clinical Pathology
That mistake set back testing for weeks and created a huge bottleneck that the nation is still grappling with. “For the governors, [testing] is really an essential tool,” New York Times reporter Katie Thomas told Michael Barbaro on his podcast, The Daily. “Think of it like a fire department that doesn’t have an essential tool like hoses. They can’t put out fires.”
As of late July, the US is testing more than 790,000 people per day, a sevenfold increase from early April. On average, California each day is testing over 120,000 people. However, the nation’s coronavirus strategy is still crippled by continuing test shortages and long lag times for results.
Supply Chain Overwhelmed
Why do test shortages continue to be an issue in the US more than four months after the World Health Organization (WHO) declared the coronavirus outbreak to be a pandemic?
Coronavirus testing is multifaceted and requires “collaboration between labs, suppliers, community sites, and hospitals,” Sammy Caiola reported for Capital Public Radio. “Any one of those pieces falling out of place can compromise county health departments’ ability to track the virus’s spread.”
Though public and commercial labs ramped up their ability to conduct and process tests in March and April, they soon ran into supply issues: swabs, pipettes, vials, and chemical reagents were in short supply around the world. “The testing supply chain wasn’t meant for this kind of onslaught of volume across the world at the same time,” Alexander Greninger, MD, PhD, assistant professor in the Department of Laboratory Medicine at the University of Washington, told the Atlantic.
And, without a national testing strategy in place, “states are duking it out for supply chains,” Blair Holladay, PhD, CEO of the American Society for Clinical Pathology, told USA Today. “It’s the wild, wild west.”
For instance, in June Sacramento County officials had to temporarily close five out of six community-based testing sites because they didn’t have enough of the chemical solution used to transport test samples to the lab, Caiola reported.
(Despite these local challenges, CHCF’s statewide COVID-19 tracking polls, conducted between March and July, consistently found that only about 1% of Californians have reported trying and failing to get a COVID-19 test in the previous week. Similarly, about 1% of California nursing home workers recently reported that residents were not able to get tested when needed.)
Rapid Testing Key to Containing the Virus
Public health experts recommend that coronavirus test results be delivered within 24 hours so those who test positive can quickly isolate themselves. “Any plan to contain the virus will depend on fast and accurate testing, which can identify newly infectious people before they set off new outbreaks, Alexis Madrigal and Robinson Meyer wrote in the Atlantic. “Without it, the US is in the dark.”
However, increased testing has strained lab capacity, which affects turnaround time. Quest Diagnostics, which is processing 130,000 COVID-19 tests per day, currently has an average turnaround time of two or more days for priority patients and seven or more days for all others. A small subset of patients may have to wait for up to two weeks to receive results, the lab said in a press release.
Long lag times for results make it extremely difficult for contact tracers to do their job.
California has no comprehensive databases showing wait times for COVID-19 test results. In mid-May, approximately 16% of primary care doctors surveyed by CHCF reported not getting timely COVID-19 test results for their patients. (Respondents ranked their responses on a scale of 1 to 5, with 1 being “not timely,” and 5 being “very timely.” The 16% accounts for physicians who ranked their responses a 1 or 2.) Among emergency department and critical care physicians in early May, approximately 9% reported that patients’ test results were not completed in a timely manner.
While waiting for their test results, people should act as if they are infected — “meaning to self-quarantine and limit exposure to others,” Phil Galewitz reported for Kaiser Health News. Health experts “acknowledge that’s not realistic if people have to wait a week or more.”
Long lag times for results make it extremely difficult for contact tracers to do their job. “Case investigators and contact tracers are often so far behind that they can’t stop an infected person from transmitting the virus to others and have to instead focus on the contacts of those who they already infected, or the individuals those people could have in turn exposed,” Taryn Luna wrote in the Los Angeles Times.
With turnaround times of up to two weeks, people who were contagious weeks before testing positive for COVID-19 may have a hard time recalling where they went or who they interacted with during those weeks.
California Health and Human Services Secretary Mark Ghaly, MD, MPH, has urged labs in California to prioritize testing turnaround for those who are most at risk of spreading the virus to others, including people experiencing COVID-19 symptoms, people who are hospitalized or in long-term care facilities, and people in institutional settings, including prisons and jails.
Wide Variations in Testing Fees
If two people get tested for COVID-19 at the same place at the same time, do they pay the same amount? Two friends in Austin, Texas, found out the hard way that the answer can depend on how you pay.
Pam LeBlanc and Jimmy Harvey went together to get drivethrough tests at Austin Emergency Center. Harvey paid $199 in cash, but LeBlanc, who presented her insurance coverage, was charged $6,408, Sarah Kliff reported in the New York Times.
“I assumed, like an idiot, it would be cheaper to use my insurance than pay cash right there,” LeBlanc told Kliff. “This is 32 times the cost of what my friend paid for the exact same thing.”
Tests should be readily available and low- or no-cost to incentivize people to be tested if they may have been exposed to the coronavirus or are experiencing COVID-19 symptoms. But an analysis by the Peterson-KFF Health System Tracker found that publicly posted price information on hospital websites ranged from $20 to $850 per single test among the 78 hospitals that provided price data. While Medicare protects patients from cost-sharing for the tests, there are no similar regulations in the private market.
California has now overtaken New York as the state with the highest case count.
Federal legislation requires insurers to cover testing without cost-sharing requirements “when the test is ordered by an attending health care provider who has determined that the test is medically appropriate for the individual.” It specifically excludes screening tests for “return to work” programs and for public health surveillance. Federal law also allows states to opt to “cover testing for the uninsured through Medicaid with 100% federal financing.” California has opted to do this.
To reduce barriers to testing for California workers, the California Department of Managed Health Care filed an emergency regulation (PDF) on July 15 that “COVID-19 testing would be classified as a basic medical necessity for health care and other essential workers, regardless of symptoms or known exposure to someone with the virus,” KQED reported. The rule took effect July 17.
California has now overtaken New York as the state with the highest case count. In the last seven days, about 8% of the 872,000 tests conducted in the state have returned a positive result, according to data from the California Department of Public Health and reported by the Los Angeles Times. WHO recommends a positivity rate no greater than 5% for at least two weeks before broad reopening occurs.
Authors & Contributors



