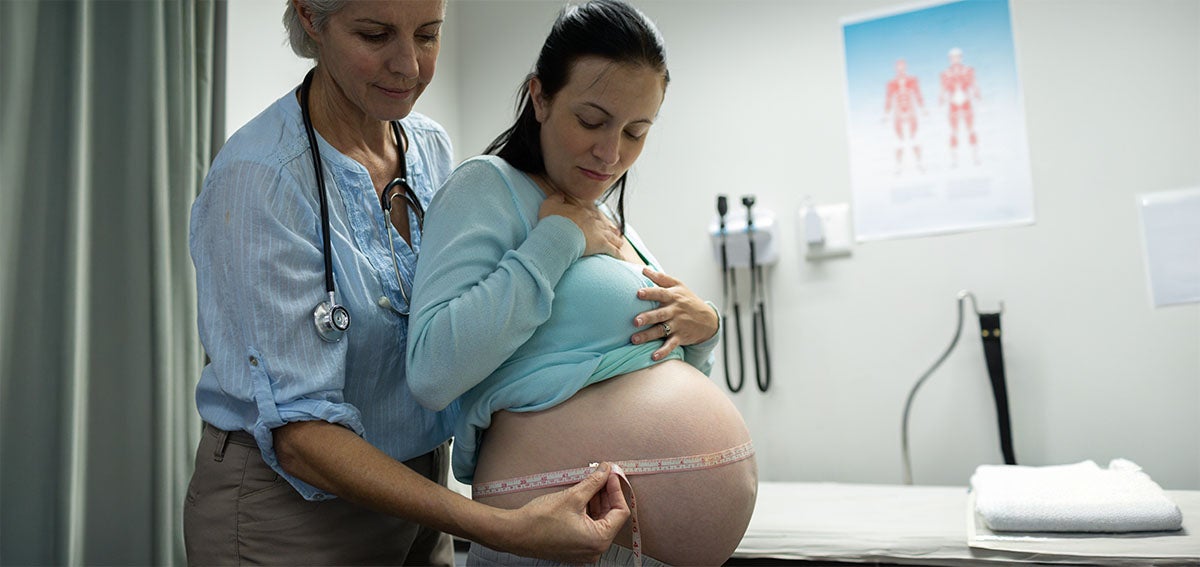
Despite an induced labor necessitated by the potential danger of preeclampsia, Morine Cebert Gators had a beautiful birth experience.

Cebert Gators, who is Black, searched diligently for a Black ob/gyn provider when she moved from North Carolina to Knoxville, Tennessee. She was mid-pregnancy, had recently finished her PhD in nursing, and was having no luck finding a doctor who looked like her. Googling and joining mother’s groups didn’t get her closer to her goal, she told Kimberly Seals Allers, host and creator of the podcast Birthright (Seals Allers’s organization, Narrative Nation, is a CHCF grantee). “I looked up my insurance provider . . . and, of course, Dr. Welch-Charles was at the end of the list.” Cebert Gators searched for her photo online. “I saw her brown skin and I was like, ‘Oh my God. Oh my God!’”
Her doctor, Shenika Welch-Charles, MD, was the only Black ob/gyn practicing in Knoxville. Welch-Charles understood the risk factors particular to women of color and flagged a potential preeclampsia diagnosis early, when routine third trimester tests detected high protein levels in Cebert Gators’s urine.
Cebert Gators gave birth to a healthy baby boy and commemorated the moment with a photo of herself with her all-Black birth team: Welch-Charles and Julia, a registered nurse, along with Cebert Gators’s husband Beau Gators and their new son, Beau Jr. The photo, which Cebert Gators shared on Twitter, quickly went viral. People chimed in with celebratory comments: “I have tears of joy in my eyes while reading your beautiful nontraumatic birth experience, which sadly should be the standard. This gives me hope!”
Maternal mortality, a key measure of public health, remains high in the US, according to the most recent data from the CDC. In 2019, 754 women and birthing people died in the US from causes related to pregnancy and birth (PDF), ranking the nation last overall among industrialized countries and on par with Uzbekistan, Moldova, and Uruguay. California’s maternal mortality rate dropped significantly from 2006 to 2013 due to concerted efforts to address key drivers. But the national rate has risen over the last decade, and disparities between Black and White birthing people remain high in both the state and nation. Black birthing people are 2.5 times more likely to die from complications related to pregnancy and childbirth than White birthing people, a racial disparity that has been reflected in the data for the past century, since records began to be kept.
For the past four years, Black Maternal Health Week has been part of April’s National Minority Health Month, an initiative to advance health equity across the country on behalf of all racial and ethnic minorities. The week of awareness calls attention to disparities in birth experiences and celebrates birthing people like Cebert Gators.
Black Maternal Health Week
This year, Black Maternal Health Week was marked with a presidential proclamation and White House roundtable discussion with Vice President Kamala Harris.
In an email interview with Nicholas St. Fleur of Stat News, Harris cited two factors, systemic inequality and racial bias, as the drivers of disparities in maternal mortality and morbidity.
These disparities cannot be explained away by differences among birthing people, such as age, income, educational level, or health insurance status. For instance, while a higher level of education is usually associated with better health outcomes, this is not the case with maternal outcomes for Black birthing people. Black birthing people with a college education have double the risk of death as their White counterparts with a high school education.
Such evidence suggests that racial bias causes the difference in death rates between Black and White birthing people. The daily stress of racism has a negative impact on the health of birthing people over the course of their lifetime. And the implicit bias of health care providers can mean that they miss the telltale signs of serious illness in their patients.
Women who speak up about symptoms aren’t always heard by their health care providers (PDF) — even if those symptoms are red flags for conditions that kill or hurt Black birthing people when they are pregnant, giving birth, or after they’ve left the hospital. Those conditions include heart muscle disease, blood clots, high blood pressure, infection, and severe postpartum bleeding, according to the Commonwealth Fund.
“When many of these conditions are identified early, there are clinical interventions that can save lives,” wrote the authors of the Commonwealth Fund report. The report estimates that two-thirds of maternal deaths in the US are preventable.
Three potential policy solutions for addressing disparities include anti-bias training, the recently reintroduced Black Maternal Health Momnibus Act, and the option for states to extend postpartum coverage in Medicaid from 60 days to a year, said Harris.
Anti-Bias Training
Harris specifically called on providers to seek out opportunities for anti-bias training. “If you are a health care provider and you are reading this, please consider getting trained or asking your employer for a training,” she said. The Biden administration recently proposed an investment of $200 million to reduce maternal mortality and morbidity. This includes funding to implement implicit bias training for health care providers.
Such training efforts are already underway in California, including the Dignity in Pregnancy and Childbirth Project, which recently launched a three-part online training course on implicit bias and reproductive justice for perinatal health providers. The free course addresses the training requirements outlined in the California Dignity in Pregnancy and Childbirth Act (Senate Bill 464). The bill, which was signed into law in 2019, requires health care providers serving pregnant people to take anti-bias training.
The course and resources were developed by Diversity Science, a professional services firm focused on accelerating progress toward diversity, equity, and inclusion in health care. (Diversity Science is a CHCF grantee.)
The training “represents a starting point on the journey to overcome racial inequities in maternal health [PDF],” said Rachel Hardeman, PhD, MPH, the project director and founding director of the Center for Antiracism Research for Health Equity at the University of Minnesota School of Public Health. “It is a critical first step from which deeper organizational and systems change must build to have real and lasting impact.”
Black Maternal Health Momnibus Act and Medicaid Extension
The Black Maternal Health Momnibus Act was reintroduced earlier this year by Congresswomen Lauren Underwood and Alma Adams, Senator Cory Booker, and other members of the Black Maternal Health Caucus. Harris was a coauthor of the 2020 version of the act when she was a senator. The package of 12 bills “would diversify the perinatal workforce, fund community-based maternal health organizations, and invest in social factors that can influence maternal health, such as access to transportation and nutritious food,” St. Fleur reported.
Harris noted that the administration’s proposed budget included funding for the Momnibus Act.
State Senator Nancy Skinner has proposed a California Momnibus Act (Senate Bill 65), which would complement the federal legislation, including extending postpartum Medi-Cal coverage to one year, requiring Medi-Cal to pay for doulas, supporting the creation of a diverse midwifery platform, and providing stipends for mothers with low incomes, among other provisions. The expansion of Medicaid (called Medi-Cal in California) for postpartum mothers is another provision of the American Rescue Plan Act aimed at improving maternal health. Medicaid pays for nearly half of all births in the US. States now have the option to extend coverage from 60 days to one year postpartum, a provision in the American Rescue Plan Act.
Earlier this month, Illinois became the first state to extend the optional coverage, which “is expected to improve health outcomes for Black mothers,” reported Alisha Haridasani Gupta in the New York Times.
California previously temporarily extended Medi-Cal for up to 12 months for women who experienced a maternal mental health condition such as postpartum depression during their pregnancy, the postpartum period, or within 60 days from the end of the postpartum period. This temporary extension will be suspended on December 31, 2021, unless the state takes additional action to extend the coverage again, temporarily or permanently.
Meeting the Standards of Care
The viral response to Cebert Gators’s birth photo was bittersweet. Every birth has potential complications, and for Black birthing people, the story doesn’t always end well, as it did for Cebert Gators.
Yet, Welch-Charles emphasized that any ob/gyn can provide the level of care she gave Cebert Gators, whether or not the provider is Black. “If you’re following the standard of care and the current guidelines, and you’re staying current, then Black women shouldn’t have bad outcomes, because those things should have been taken care of from the very beginning,” said Welch-Charles.
Authors & Contributors

Heather Tirado Gilligan
Heather Tirado Gilligan is a journalist who has written for publications including Slate, The Nation, CNN, and the Washington Post. Previously, she was executive editor of the California Health Report, a news nonprofit covering disparities in health and access to health care. Heather received a master’s degree in journalism from UC Berkeley and a PhD in English from Rutgers University, where she studied race in American culture.