When people think of chronic health conditions, they often think of diabetes or heart disease. But alongside these physical conditions, mental health disorders are among the most common chronic illnesses that people face, both in the United States and here in California. Among adults statewide, nearly one in six experiences a mental illness of some kind in any given year. One in 24 has a serious mental illness resulting in functional impairment that limits activities of daily life. Children and teenagers also experience mental health disorders at high rates: 1 in 13 has an emotional disturbance that limits participation in regular activities. And while mental illnesses generally can be managed successfully, too many people miss out on treatment.
CHCF is committed to advancing care for people with mental health disorders and to supporting the ability of California’s safety-net system to provide care for mental illness just as it does for physical needs. Using the most recent data available, the CHCF report Mental Health in California: For Too Many, Care Not There offers a broad overview of mental health in California, including prevalence of illness, suicide rates, supply and use of treatment providers, and mental health in the correctional system.
As in many other policy areas, the statewide averages mentioned above mask deep disparities. The report finds significant differences by race and ethnicity, region, and income, as seen in the charts below.

Another area of tremendous difference is in suicide rates. The rate in the Northern and Sierra region is nearly triple that of Los Angeles County.

Troubling trends in adolescent depression are also notable. In 2013, the last time CHCF compiled prevalence data for mental health conditions in California, about 1 in 12 teens reported experiencing a major depressive episode in the past year. Now, it’s one in eight — a 50% increase.
Trouble Accessing Treatment
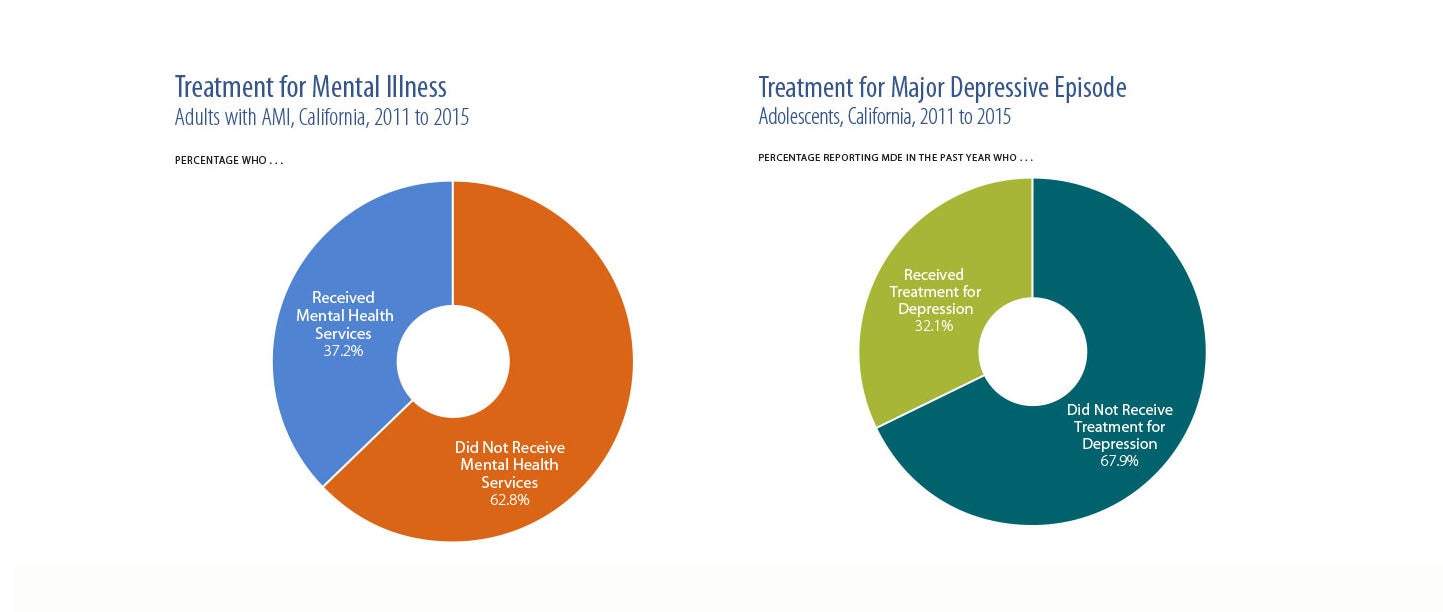
Federal and state mental health parity laws and the Affordable Care Act (ACA) have greatly expanded private and public insurance coverage for mental health conditions. Last summer a statewide poll that was supported by CHCF found that three out of four Californians believe this coverage is important — and that treatment of mental health conditions can help people live healthy and productive lives. Yet, despite the availability of coverage and belief in its effectiveness, access to care remains a challenge for many people. The report shows that nearly two-thirds (63%) of adults with a mental illness do not receive treatment. Of the one in eight teenagers with depression, only about one-third (30.5%) receive treatment. One bright spot is adults with a major depressive episode — nearly two-thirds of adults with the condition receive treatment.
California lacks an adequate workforce to meet the needs of Californians with mental health conditions. Last month, the Healthforce Center at UCSF published California’s Current and Future Behavioral Health Workforce, in which researchers identified significant variation in the distribution of mental health care providers across regions of the state, leaving areas with the greatest need with the fewest providers. In addition, a large share of psychiatrists and psychologists are expected to retire in the next decade. California must make “substantial investments” to meet future needs for behavioral health professionals, the writers concluded.
California can and should do better in providing treatment for those who need it. We are fortunate to have state policies that support access to both insurance and care. We also have a rich source of funding in the Mental Health Services Act (MHSA), which will raise nearly $2 billion this year through a 1% tax on incomes over $1 million. Most of the money is delivered to county mental health programs to expand community services. At the state and local levels, conversations are ongoing about how these and other mental health dollars can best be spent. Local communities are taking advantage of opportunities within the Medi-Cal program to better integrate behavioral health care, including the Whole Person Care Pilot program, which is developing integrated models of care for people with multiple needs — many with mental illness.
Data Gaps
While this report compiles compelling data from multiple sources, it also highlights the data we lack. First: outcomes. We don’t have sufficient information about how people receiving mental health services in both the public and private systems actually fare. Medi-Cal is starting to track how children in the Medi-Cal mental health system are functioning at home and in school, and Assembly Bill 470, passed last year, requires the Department of Health Care Services (DHCS) to measure disparities in access and outcomes. These efforts are in the early stages and much more work is needed. Second, we need to understand more about what the mental health crisis looks like for adolescents. Generally considered healthy by the medical care system and so not a traditional focus of attention, California’s young people have high rates of depression and are likely to go untreated.
Taken together, the many charts and graphs in this report highlight the need for better care for people with mental health issues. We hope researchers and policymakers statewide can use this work to inform projects designed to improve both access to treatment and outcomes.
Authors & Contributors






