
Since the COVID-19 pandemic began, residents of the Central Valley’s Kern County have landed inside Kern Medical in nonstop numbers — and it isn’t only because local case rates have been consistently higher here than in other parts of the state. People are rushed to the hospital’s trauma center after crashing cars, attempting suicide, or experiencing domestic abuse or other forms of violence.
“A lot of terrible things have happened in our county that people don’t know about,” said Scott Thygerson, CEO of Kern Medical, a regional public health care system with a 222-bed hospital in Bakersfield, 1,800 employees, and a full range of outpatient services.
Historically, such tragedies spike in the summer, but trauma season has been year-round since the onset of the pandemic.
“Traumas went through the roof almost immediately [when the pandemic hit],” said Thygerson. “Within the first month, we went from 235 trauma activations a month to 290. It has not stopped or slowed down since.”
“Patients in need of psychiatric care are overwhelming the hospital’s emergency department, and they have filled Kern Medical’s inpatient psychiatric unit.“
As a result, Central Valley patients have found themselves in one of the busiest trauma centers in the state and the only one between Los Angeles 115 miles to the south and Visalia 80 miles to the north.
No Letup in Demand for Care
The need for more help in caring for the region’s population is not subsiding. In response, Kern Medical has stepped up efforts to recruit new employees at every level and to fill the training pipeline with future health care workers.
Non-trauma patients of all ages at Kern Medical are acutely ill with conditions unrelated to COVID-19. Thygerson believes delayed care during the pandemic may be driving some of these admissions.
“We are running double our ICU levels, and we have a lot of sick babies,” said Thygerson. “The neonatal intensive care unit is full.”
Patients in need of psychiatric care are overwhelming the hospital’s emergency department, and they have filled Kern Medical’s inpatient psychiatric unit — the only one housed in an acute care hospital in the region.
Many more patients struggling with mental health problems are showing up at the 10 Kern Medical outpatient clinics that dot the county.
“Nurses are physically exhausted, they’re mentally exhausted, and they’re not exempt from dealing with a lot of the same issues our patients deal with.“
—Paula Isbell, RN
“We’ve seen a huge increase in patients scoring higher for being at risk for potential suicide,” said Natalee Garrett, vice president of strategic development at Kern Medical. As part of a standard screening process, patients complete a questionnaire on how they feel before they see a provider. For patients scoring high on the survey, psychologists also see them on the spot. These interventions are occurring at a record pace.
“Patients are so fragile, and they need attention now,” said Alicia Gaeta, a nurse at Kern Medical. “They don’t have three weeks to wait if they’re having a crisis. We make sure they don’t leave the room without talking to a psychologist and getting help.”
Responding to Staff Attrition
While patient demand has soared without interruption since the start of the pandemic, Kern Medical’s complement of nurses and other health care workers has thinned.
“Nurses are physically exhausted, they’re mentally exhausted, and they’re not exempt from dealing with a lot of the same issues our patients deal with,” said Kern Medical registered nurse Paula Isbell. “They have to deal with all their struggles — getting sick, divorce, custody issues — put their scrubs on, act like everything’s fine, and take care of someone else’s life while their own is falling apart.”
Isbell said the pandemic has pushed some nurses to leave the profession altogether. Others have departed Kern Medical for lower-stress, higher-paid work they can do at a school or an insurance company.

Kern Medical has had to depend heavily on more-expensive traveling nurses, many provided by the state.
“Thank goodness the state has been sending travelers. And thank goodness the state is providing financial support for those nurses. As a safety-net hospital, without this support, we would face significant issues,” said Thygerson.
Vital Work of Medical Assistants
Many other heroes have provided care during the pandemic, such as medical assistants who support patients and physicians in its busy outpatient clinics.
“We do everything on the back end for the doctors and advocate for patients,” said Erika Guerrero, a medical assistant in one of the clinics. “And we’ve been working like crazy.”
“Medical assistants perform a vital job and work very, very hard,” said Renee Villanueva, chief ambulatory and outreach officer at Kern Medical.
Their commitment to their patients can be very personal.
“I love the patients that we serve. Many are the patients that no one wants to listen to. They may not have any money. And they need our help,” said Guerrero. “And me, coming from that background, I was that little girl, that teenager who grew up in that atmosphere. I know how it feels to be that person.”
“For Kern Medical, an effective pandemic recruitment strategy is to continue bringing nurses in for face-to-face interviews and tours.“
Like public health care systems across the state, Kern Medical has tried to buoy staff spirits. Maintaining a positive work environment in the hardest of times “is not about the materialistic things,” Guerrero said. “It’s not about ‘we’ll give you this.’ No, it’s about the support. If I need anything, it doesn’t matter if it’s Sunday night, I can call my supervisors anytime, and they are amazing.”
In interviews, Kern Medical nurses, medical assistants, and care coordinators say they have grown closer to their colleagues during the pandemic, which may have helped to diminish burnout. “They talk things through a lot with one another, and I think that’s how they kind of decompress,” said Garrett.
Isbell believes this deep loyalty to coworkers and “knowing that for you to leave would be devastating to them” is what keeps many nurses on the floor.
“There are days when it’s so much easier to just worry about myself,” Gaeta said. “Then I see how hard everyone’s working, and that encourages me to keep going.”
Overcoming a Longstanding Shortage of Health Care Workers
Before the pandemic, Kern Medical sometimes struggled to attract and hire doctors, nurses, licensed vocational nurses, medical assistants, respiratory therapists, and others. A chronic shortage of health care workers exists in the Central Valley, and the public safety-net hospital has struggled to pay salaries that compete with nearby health systems.
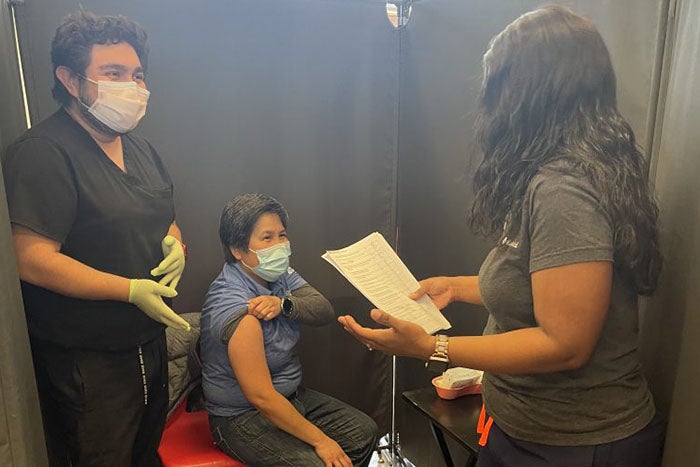
For Kern Medical, an effective pandemic recruitment strategy is to continue bringing nurses in for face-to-face interviews and tours so they can get a better feel for the hospital’s learning atmosphere and tight-knit team.
“Once we get them in here, we have the opportunity to let them know that we’re going to support them, and we are going to foster a warm work environment,” said Isbell. Several nurses told her that other employers don’t provide the in-person opportunity, which helped them decide to accept the hospital’s offer.
Student Opportunities
Another long-standing recruitment strategy, which was in place before the pandemic, also focused on bringing in potential future staff, including high school students, to see the system in action.
As part of the Health Careers Academy run by the Kern High School District, 40 to 50 students who expressed interest in health care came to Kern Medical each day to shadow medical staff, observe procedures, and perform clerical work. That was how Garrett, one of Kern Medical’s leaders, started her health care career as an academy participant from 2003 to 2005.
Given the significant need for more medical assistants and potential applicants right across the street at East High, Kern Medical partnered with the school to develop a medical assistant program.
After being postponed in 2021 by the pandemic, the program is expected to resume in the fall. Students will continue to learn hands-on patient care at the hospital and clinics and to complete coursework. After graduation, they can take the exam to become a certified medical assistant.
“It does not cost students anything compared to private training programs that may charge as much as $16,000 to $20,000 to become a medical assistant through these private colleges,” said Garrett. “They could have a job right after school with us. They would already know our systems, and we could onboard them immediately after graduation.”
Kern Medical’s focus on who it recruits is core to retaining staff. “Getting the right people is so crucial. We attract people who have a passion for what they do,” said Garrett. And many of these students who start as medical assistants further their training in the medical field to become nurses, pharmacists, computer engineers, and other health workers, with Kern Medical’s support.
Like all of California’s public health care systems, during the pandemic Kern Medical has expanded its traditional role of caring for the most vulnerable — all the while executing well-developed plans to welcome a new generation of health care heroes.
This article was adapted with permission from the California Association of Public Hospitals and Health Systems (CAPH), which published its story on February 10. Copyright © 2022 CAPH. All rights reserved.
Authors & Contributors

Aisling Carroll
Aisling Carroll is a Bay Area–based freelance writer and former journalist who covers health care, digital health, hospitals, and the patient-doctor relationship. Her work has been published in Stat News, HuffPost, Business Insider, Congressional Quarterly, and others. Carroll received a bachelor’s degree in political science from UC San Diego.





