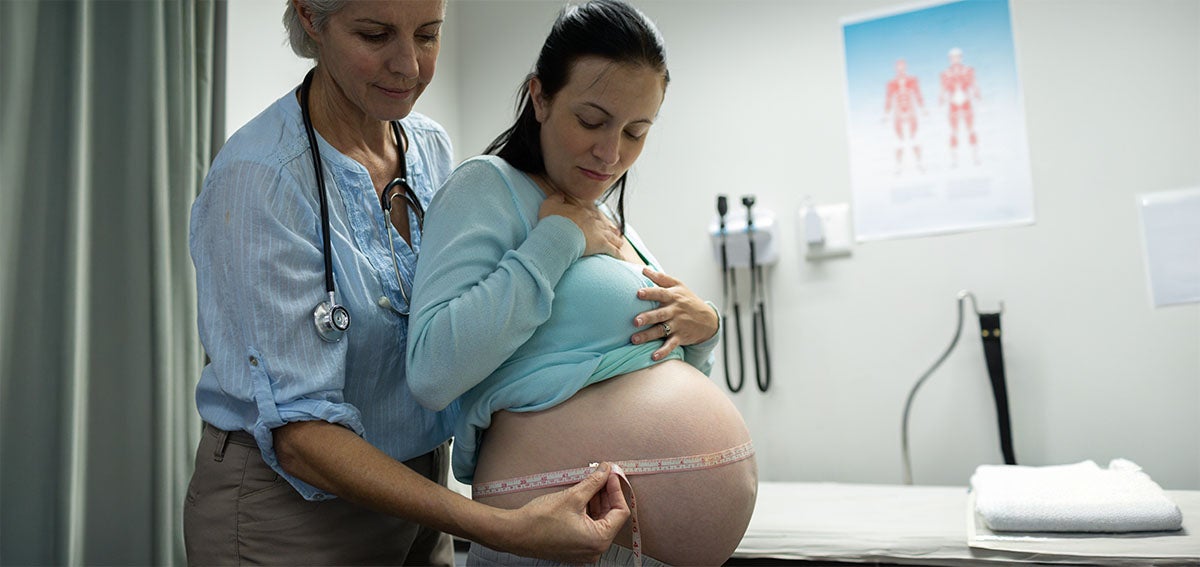
During her last pregnancy in 2020, Tanefer Camare was determined to find a midwife in her community and give birth at home. “Given my history, I knew that was my best option,” said Camare, a 40-year-old Black mother of four living in the Bay Area. Camare experienced labor and delivery at a hospital when she gave birth to two of her babies. While there were no complications, she felt she had little control over the process. In contrast, at home with a midwife, she said, her labor was easy. “She made me feel more comfortable and was open to talk and listen — I felt that she understood me,” she said.
“I understood that the system of hospital birth is already a risk to me as a Black woman,” said Camere, who expected a battle when she opted to have her first baby at a hospital. “They assume that you don’t know anything about your body and that they know what’s best for you. They apply general understanding and not what is specific to you.”
In contrast, midwifery care involves building a relationship of trust between the provider and the birthing person, with both sharing the decisionmaking around the birth. During a home birth or a delivery at a birthing center, midwives support and spend more time with birthing people and focus on the individual experiences and struggles that influence their clients’ lives.
“This is very difficult to do in a hospital setting,” said Kimberly Durdin, CPM, LM, IBCLC, a midwife and co-founder of Kindred Space LA, the only Black-owned birth center in South Los Angeles and a hub for midwifery care. “In hospitals, women have to fight to be allowed to walk, move around, have family members present, and honor the timing of birthing as a natural process.”
Yet, for Durdin it is not a question about whether to deliver in a hospital or a birthing center or at home. “It’s about giving more opportunities for people to have a choice before, during, and after giving birth,” she said.
Growing Role of Midwives
Midwives assist people with low- to moderate-risk pregnancies like Camare and are a growing component of the maternity workforce in California. Known for a whole-person approach, they view birth as a natural physiological process and provide comprehensive care before, during, and after the baby is born. There are approximately 1,200 certified nurse midwives (CNMs) and 500 licensed midwives (LMs) in the state (PDF). CNMs are registered nurses with graduate training from an approved midwifery program, and they practice mostly in hospitals. LMs are trained in approved three-year programs and practice in birth centers and homes.
The number of births attended by midwives in the state has risen in the last 15 years, and documented outcomes show that midwifery care is as good as or better than hospital care provided by obstetricians. For example, studies have found that midwifery care results in fewer episiotomies; lower rates of cesarean sections , complications, and interventions; increased rates of breastfeeding; and higher patient experience scores, according to a series of articles published in The Lancet. With fewer interventions, midwifery can also contribute to lower health care costs.
The Maternity Care Workforce
California needs more midwives to help solve the growing shortage of qualified maternity care clinicians, including obstetricians. Additionally, the existing maternity care workforce fails to reflect the diversity of the state.
“There are catastrophic disparities, particularly in childbirth,” said Kim Dau, RN, MS, CNM, director of the nurse-midwifery program at the UCSF School of Nursing. “In California, 87% of nurse midwives identify as White, which doesn’t match the demographics of the state,” she said. The racial and ethnic differences between providers and patients have an impact on the entire birth experience, from prenatal to post-partum, she said. “There is a lot of work to do.”
Dau also co-leads the Midwifery Mentoring and Belonging Program, a collaboration between schools of nurse-midwifery at UCSF and California State University, Fullerton. The other co-leaders are Amber Bell, CNM, MS, and Asmara Gebre, CNM, MS, at UCSF; and Angela Sojobi, RN, BSN, MSN, DNP, at Cal State-Fullerton. The mentoring program, which is funded by CHCF, pairs midwifery students who identify as Black, Indigenous, and/or people of color with midwives of color. The overall goal is to provide the support that many providers of color say is needed to ensure that students of color stay in the field, increasing diversity in the midwifery workforce. It is not easy, Dau said. “My ability to educate a more diverse group of midwives will depend on my ability to attract diverse faculty, and right now there is very little incentive,” she said.
Unlike other states, California doesn’t provide financial support for clinical sites to take in midwifery students. “Education opportunities for midwives are limited,” Dau said. The only licensed midwifery program in California closed at the end of 2022. Operating a training program is expensive, and integration of midwives in health care systems continues to present challenges.
Legislation to Build the Pipeline
As part of the 2022-23 state budget, Governor Gavin Newsom and the Legislature included funding to allow midwives to participate in the Song-Brown Program, which aims to increase the number of students and residents receiving quality primary care education and training in areas of unmet need throughout California. “While the funding is still not sufficient, this is a huge milestone,” said Holly Smith, health policy chair at the California Nurse-Midwives Foundation.
While supporting expansion of the midwifery pipeline will increase access to care, reduce costs, and improve outcomes for birthing people and their newborns, the shortage of providers and lack of provider diversity are not the only obstacles. Ideally, low-risk pregnancies and deliveries, which account for the overwhelming majority of births, would be managed by midwives, while moderate-risk cases would be overseen by physicians and midwives jointly. That would leave the high-risk cases to be managed by obstetricians.
However, the prevailing model of maternity care in the US relies on obstetricians, who are trained to treat the highest risk patients, to be the central providers of maternity care for all types of pregnancies.
Doctors perform critical, lifesaving procedures for many pregnant people, Durdin said. “We need ob/gyns and hospital care, but the current model of care by ob/gyns in hospitals is a mismatch for low-risk women,” she said. As a result, hospitals often use unnecessary and costly interventions that frequently lead to more interventions and poor outcomes.
The widespread use of epidural analgesia is a good example of the cascade of intervention. While epidurals can provide effective pain relief during labor, other modalities, such as water immersion or freedom of movement could provide the needed relief. Epidurals are not needed in most low-risk births, and they can lead to a sudden drop in blood pressure, longer labor, difficulty moving about, difficulty pushing the baby out, fever, or other problems.
In 2020, efforts to advance midwifery in California paid off with the enactment of SB 1237, which removed the requirement that CNMs be supervised by a physician and created an independent scope of practice for this class of midwives. “This legislation is very important but only a first step,” said Kathleen Belzer, founder and co-chair of the California Nurse-Midwives Association, the bill’s sponsor.
While the legislation addresses the difficulty midwives face in finding a supervising physician, the state has yet to update the regulations needed to comply with the bill. SB 1237 also preserves the ability of nurse-midwives in any setting to collaborate with physicians in the co-management of patients with complications who need services that fall outside the independent scope outlined in the bill. For licensed midwives, physician supervision has not been required since the enactment of AB 1308 in 2013.
Birth Preferences Overlooked
Listening to Mothers in California, a statewide survey about the maternity concerns and outcomes of women and birthing people, provides relevant findings. While the vast majority of birthing people said they used an obstetrician for their prenatal care and births, over half said they would want (17%) or consider (37%) a midwife for a future pregnancy.
According to the survey, produced by the National Partnership for Women & Families with support from CHCF and the Yellow Chair Foundation, health providers often disregard people’s birth preferences, increasing the risk of death and complications for them and their babies. Black birthing people are the least likely to be listened to. In California, they are four to six times more likely to die (PDF) from complications related to pregnancy and childbirth than people in all other racial/ethnic groups. Black birthing people are 2.5 times more likely than White people to experience a severe maternal complication. Although Black people represent only 5% of California’s birthing population, they account for 20% of the state’s maternal deaths.
Antoinette Coleman is a 32-year-old mother of four in Fairfield, California, who received care from an ob/gyn in the hospital when she had her first two babies and a midwife at home with the other two. “Care with midwives is more personal, while the care at the hospital is very fragmented, sterile, cold,” she said. “Once the baby is out of your body, you don’t count anymore.” When she had questions after one of her hospital births, she says she was told by hospital staff that she was no longer under their care and to see her primary physician.
An increasing number of birthing people prefer to receive care from midwives, but many face significant barriers to accessing that care. While Medi-Cal covers midwifery services, the requirement doesn’t apply to private insurers, many of which may not admit midwives to their provider networks or cover midwifery care at all. Midwifery has come a long way in California, but challenges remain, including support from the medical community, obstacles to midwifery care reimbursement, and variable availability of hospital contracts.
“Medi-Cal does cover midwifery services, but unfortunately reimbursement rates are extremely low and not enough to sustain a practice,” Durdin said. “The Medi-Cal system is very difficult to be enrolled in as a provider, and it’s even more difficult to actually get paid. We want to offer this option of payment to our clients but find that it does not create sustainability for our business model.”
“Not Just a Medical Event”
At Durdin’s Kindred Space, where midwives prepare pregnant people physically and emotionally for the birth experience, 15 to 20 people per month receive this personalized, intensive care. Midwives usually know more about their clients’ history than providers in hospitals and can determine needs related to personal finances, anxiety about COVID-19, or mental health issues. The center identifies the services their clients need in the community, including an eight-week mental health program the center funds. Durdin’s nonprofit Birthing People Foundation provides free and low-cost education, training, and certification to empower people of color and address maternal and infant health disparities.
“Midwifery care is about the whole person, and the care provided by Kindred Space LA focuses on the larger context into which the baby is being born,” said Stephanie Teleki, who coleads CHCF’s maternity care work. “It’s significant that the midwives address the non-medical circumstances of life that influence the health of a parent and child. The birth of a human is not just a medical event — it’s a life-altering experience that needs a village. Somehow, we have lost that truth in our society, and the reinvigoration of midwifery at this time is partly about reclaiming it.”
Durdin has set a standard for achieving that vision.
“We have created what we want for ourselves,” she said. “We are mothers, and we feel called to do this knowing we are inspired by the countless midwives who delivered babies over hundreds, if not thousands of years before hospitals existed.”
Authors & Contributors

Silvina Martinez
Silvina Martinez is a public relations consultant specializing in health care and multicultural communications. A former newspaper reporter in Latin America and California and a medical interpreter herself, she works on health care initiatives and policies designed to expand access to care as well as educate and empower patients to take control of their health.

Christian M. Beckley
Christian M. Beckley is a Los Angeles-based birth photographer and videographer who also is a perinatal/postpartum specialist and a lactation specialist.
She has worked in these disciplines for more than five years and loves documenting families on their journeys to parenthood.