|
Getting your Trinity Audio player ready…
|

Carolina Ajca, the lead physician assistant for the Healthcare in Action street medicine team in San Bernardino, knocks on a client’s motel room door to wake him for his medical checkup. Photo: Zaydee Sanchez
Two years ago, Jennifer was pregnant, living in a tent with her boyfriend in San Bernardino, and addicted to methamphetamine. Today, she is vibrant, sober, mentally sharp, housed, and employed as a Medi-Cal In-Home Supportive Services worker.
The reason she and her baby are alive today is that Hannah Cutino, a member of Healthcare in Action (HIA) mobile street medicine program, wouldn’t give up on her. “Hannah is solid, the most solid person I know,” Jennifer said. “I’d refuse help. I’d vanish and then she’d find me. She’d get me food.” Cutino even delivered a leash and harness for Jennifer’s dog.
“Finally, I gave in,” Jennifer said. “I knew I needed help. It just took a lot to trust that anyone would want to help me.”
Rebuilding a Troubled Life
The HIA health care providers were able to offer Jennifer immediate medical attention from their fully equipped medical van, which visited her encampment regularly. They continued to see her for added support, and that included swiftly connecting her to mental health services through San Bernardino County and prenatal care with a local OB-GYN. After ups and downs, Jennifer ultimately entered detox and a sober living facility — and she gave birth to a son, who is living with relatives. Now she is living in an apartment.
Because she’s mentally stable, Jennifer, 40, can visit her son, which has fired her dreams of regaining custody of him. As she rebuilds her life, HIA continues to provide consistent care for Jennifer, including medication for depression. When HIA can’t provide a needed service, Cutino and the team figure out who can. They’ve connected Jennifer with a therapist she sees regularly. Jennifer says Cutino and the team are anchors for her mental health and well-being. In addition to serving as health care providers and advocates, they deliver encouragement and moral support.
Homelessness can significantly worsen substance use and mental health problems by making it more difficult for people to reduce or quit using and complicating their efforts to access treatment, according to the California Statewide Study of People Experiencing Homelessness from the UCSF Benioff Homelessness and Housing Initiative. The study looks comprehensively at causes and consequences of homelessness.
“Many who experience homelessness have had past trauma,” the study found. “The experience of homelessness is highly stressful — exposing participants to worry, poor sleep, violence, and hopelessness. Mental health problems can increase one’s risk for homelessness and be exacerbated by homelessness.” More than 181,000 people in California were unhoused in 2024. Two-thirds of this population report that they faced a mental health condition and about half reported having at least one complex behavioral health need such as drug or alcohol use, current hallucinations, or recent psychiatric hospitalization, according to the UCSF initiative. Twenty-eight percent wanted substance use treatment but were unable to obtain it.
“We are seeing an enormous health equity gap and unmet health care need,” said Michelle Schneidermann, MD, director of people-centered care at the California Health Care Foundation. “Street medicine is uniquely positioned to close this gap, meet the patients where they are, and deliver the care they so badly need.”
I knew I needed help. It just took a lot to trust that anyone would want to help me.
Jennifer, who is in recovery and recently moved to temporary housing
HIA is part of the SCAN Group, a nonprofit, integrated care delivery organization that includes a Medicare Advantage plan and other services aimed at seniors and underserved populations. HIA is active in Los Angeles, Orange, Riverside, San Bernardino, San Diego and San Mateo counties. Depending on the location, HIA might contract with health systems, hospital systems, municipalities, managed care organizations or community-based organizations. The presence of behavioral health care services in a street medicine team can substantially improve the odds of success.
Visiting Encampments
In the Inland Empire, which includes Riverside and San Bernardino Counties, HIA contracts with Medi-Cal managed care providers Molina and Inland Empire Health Plan, the nation’s largest nonprofit Medicare-Medicaid public health plan with more than 1.5 million members.
HIA began its efforts in the Inland Empire in 2023 led by physician assistant Eddie Menacho. Menacho asked Kristen “Red” Malaby, then a community volunteer, to introduce him to people living in local encampments. For months Menacho loaded his backpack with medical supplies and tagged along with Malaby as she made her rounds to deliver food, water, and clothes to people in need. He dispensed much-needed care and medication. Over time, he came to understand that Malaby, a single mom, had troubles of her own.
“I’d had a major shoulder injury,” she said. “Jobs that I used to get, I stopped getting because I was disabled. At one point, I was in danger of losing my own housing.” She now supervises all the peer navigators — in effect, case workers — most of whom have lived experience with housing insecurity, disability, or substance use and mental health issues.
Peer navigators are paired with doctors, physician assistants, and clinical support staff and visit encampments, riverbeds, streets, and parks where unhoused people live. They deliver care from backpacks loaded with supplies or from their fully equipped vans — whatever it takes. HIA teams operate with the mandate to reduce human suffering, said Benjamin Kaska, HIA’s chief of integrated care delivery.
According to Kaska, in 2025 HIA served nearly 7,000 people. HIA stands out for its integration of three key pillars: clinical services, housing navigation, and Enhanced Care Management (ECM) — a state initiative designed to address both medical needs and the social drivers of health, such as housing and food insecurity. By supporting patients’ clinical, social, and housing needs in a coordinated way, HIA aims to help patients achieve long-term stability.
Long-Acting Care
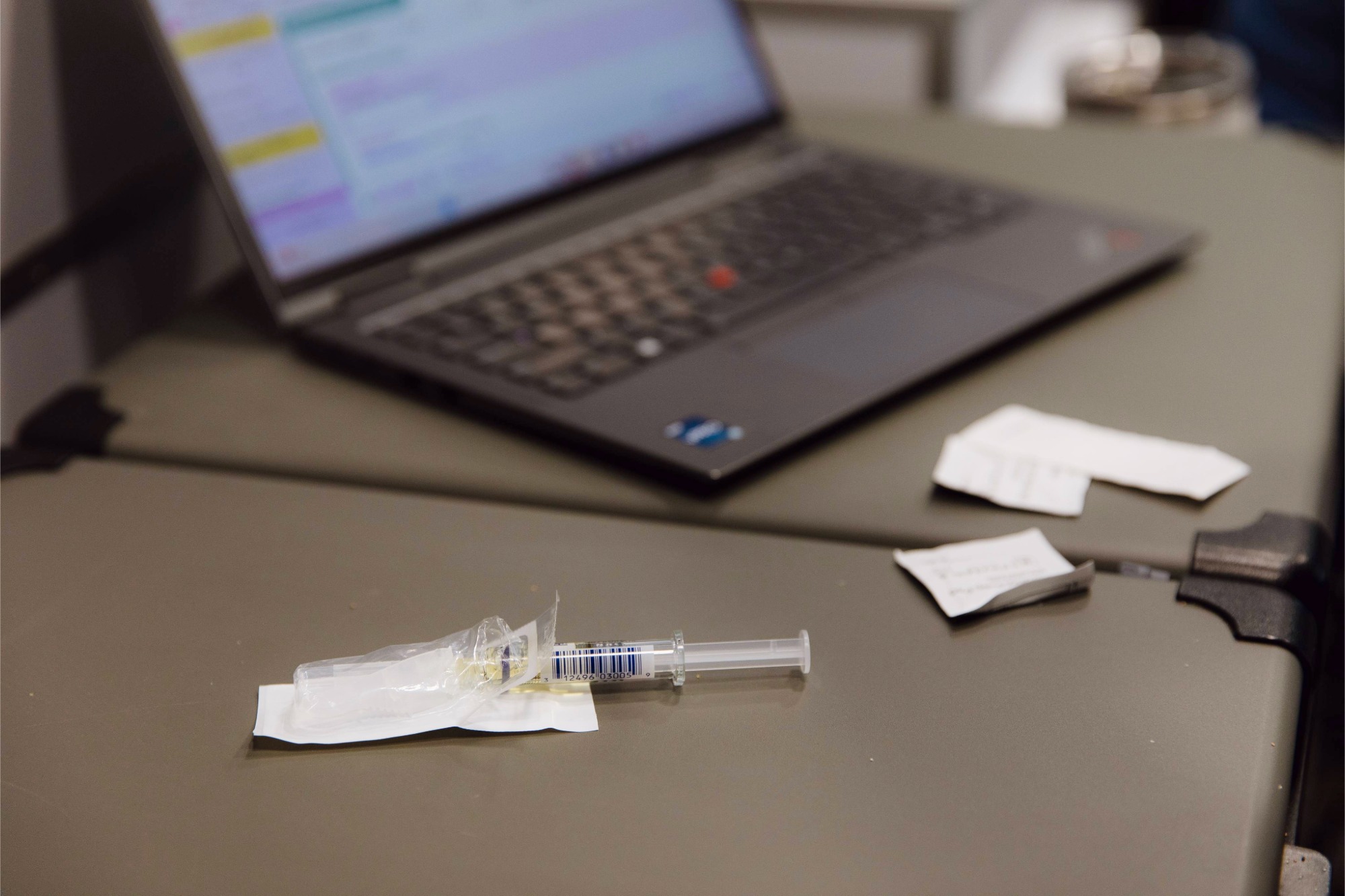
The health care teams provide treatment for substance use disorders, mental illnesses, medical diagnoses of acute and chronic illnesses, wound care, routine checkups, and more. For patients with behavioral health issues, a key element of this care is the use of long-acting injectable substance use disorder and mental health treatments. The long-acting injectables often work better for people who lack transportation and live in unstable conditions; there are no clinics to visit or daily pills to lose, have stolen or forget to take.
These tools have been lifesavers for 26-year-old Bryce, who now receives long-acting injectable buprenorphine to manage pain and treat opioid use disorder. The practitioners also inject long-acting aripiprazole to treat his major depression. Peer navigator Syvannah Butler met Bryce when he lived at an encampment near the I-210 freeway in San Bernardino.
Bryce was in bad shape. After he was struck by a train last year in Riverside, doctors amputated both legs above the knee, and his hands were badly hurt with significant loss of function. After four months in a hospital, Bryce returned to the streets with open wounds and without adequate pain management.
“At first I would just blow off Syvannah because I wanted to keep getting high,” Bryce said. “But they kept coming back.” The HIA team offered wound care, food, clothing — anything to build trust. While Bryce worked on his sobriety, the team secured a voucher for temporary housing in a nearby Motel 6, where he currently lives.
Everything helps more than I thought it would.
Bryce, now living in temporary housing at a hotel as he recovers from amputation of both legs
Bryce uses handles on the van door to hoist himself up from his wheelchair into a seat. HIA clinical support partner Stephanie Morales checks his blood pressure. Physician assistant Martha “Caro” Ajca speaks to Bryce gently, and injects long-acting medications into his stomach flesh. The shots are painful and sting badly afterward, he said, but they are the only thing that works. “With methadone you have to get up and go to a clinic every day, and that’s really hard for me,” he said.
“Are you hungry? We can get you something to eat,” Ajca said to Bryce. The team picks up food from a Taco Bell restaurant next door, and they deliver it to his room. “This is what our patients need,” she said. “They need this family-like relationship with us.”
‘Nothing Good Comes Easy’
Bryce was smiling, something that never happened when HIA began providing care to him. “Everything helps more than I thought it would,” he said. Thanks to HIA, he recently was fitted with prosthetic legs, and now he receives physical therapy. “It’s hard to balance with the prosthetics, but I’ll get it,” he said. “Nothing good comes easy. Sometimes the hardest things you do are the best things.”
Bryce’s state disability claim was recently denied, which leaves him with no income — a major barrier to eligibility for permanent housing. With HIA’s help, he’s appealing. For the first time in a long while, he sees options. “What I’d really like is to get a job someday,” he said. “I’ve been told I’m great with people.”
A few miles away, Jorge, 33, met the HIA van outside his studio apartment before he headed off to work at a deli and attend a school where he’s learning to install and repair HVAC systems. Jorge served seven years in prison for crimes related to his history of substance use. He said he has used intravenous methamphetamine since age 14. Because he has been diagnosed with bipolar disorder, the HIA team gives Jorge a monthly long-acting injectable antipsychotic, as well as long-acting injectable naltrexone to manage opioid use disorder. They also deliver his other prescription medication and have connected him with an outpatient rehab program, where he attends group therapy.
Compassion: Mandatory
Jorge said he’s grateful to HIA lead peer navigator Robert Mora, who found him living on the streets. After Jorge stopped using, he had to take care of some unfinished business. An outstanding warrant compelled him to serve 60 days in jail last summer. “As soon as I was out, I called Robert. I knew I needed to get the injectables or I wouldn’t last.”
“His call made my day — or maybe my month,” said Mora.
That comment doesn’t surprise HIA lead physician Timothy Ibrahim, MD. “This is not a job. This is something more,” he said. HIA teams serve individuals many people cross the street to avoid. Compassion is mandatory.
Most of the people they serve are victims of major childhood trauma, abuse, neglect, sexual victimization, homelessness as youth, and more, Ibrahim said, adding that homelessness, mental health challenges, and substance-use disorders accompany and complicate their problems.
The work is challenging, Ajca said. “But this is also some of the most gratifying work anyone can do. We see lots of wins.”
When Jennifer finishes her appointment with Ajca, she collects her prescriptions for depression and high blood pressure, exits the van, and gives team members a hug. “They are family,” Jennifer said. “Because of them, I now have a chance at life.”